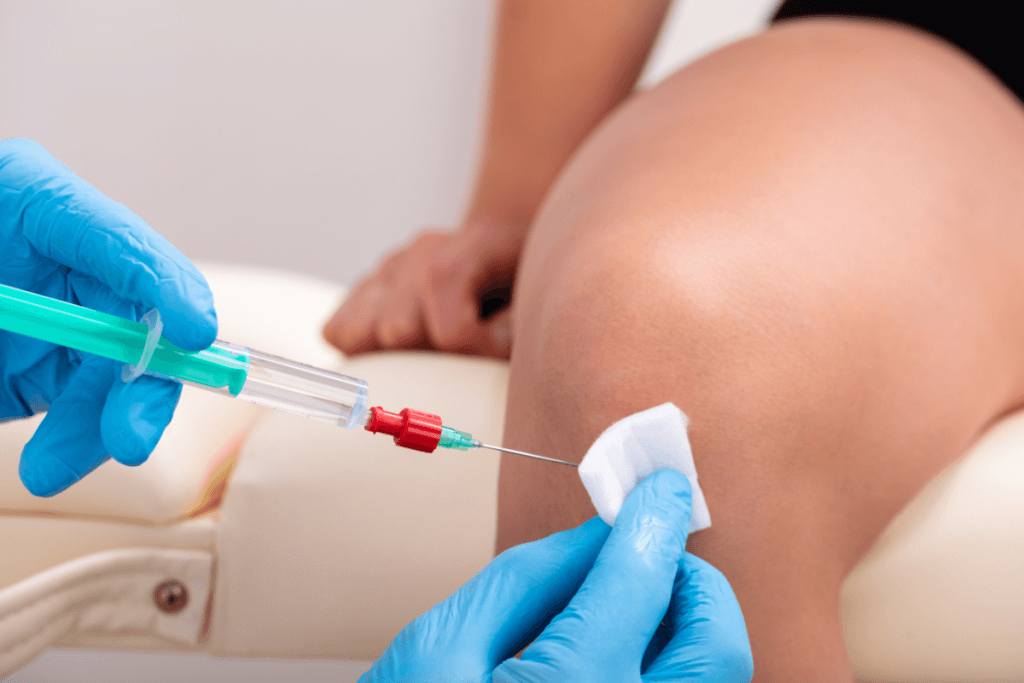
Monovisc knee injection is a hyaluronan viscosupplement used as an intra-articular option for selected patients with knee osteoarthritis, and clinics usually evaluate it through five lenses: indication fit, safety, aftercare, documentation, and payer policy. For care teams, the value is less about a headline claim and more about operational fit. It uses a single-injection format, so patient selection, procedure-day counseling, and chart completeness matter from the first visit.
That makes a clinic-facing review useful. Teams often need to confirm where it fits after conservative therapy, what to watch for after administration, how to standardize discharge advice, and why coverage may be denied even when the diagnosis is clear. The sections below focus on those practical questions without turning the topic into a product sheet.
Key Takeaways
- Single-injection format can simplify scheduling, but it raises the stakes on upfront screening and counseling.
- Use should align with current labeling, clinic protocol, and payer criteria for knee osteoarthritis.
- Most tolerability issues are local and short term, but red-flag symptoms need prompt review.
- Aftercare works best when activity limits, return precautions, and follow-up steps are written and standardized.
- Coverage often depends on clear documentation of diagnosis, prior conservative care, laterality, and product details.
Monovisc Knee Injection: What It Is and Where It Fits
Monovisc is a hyaluronan product used for viscosupplementation, meaning it is placed into the joint to supplement the synovial environment. In plain language, it is a knee gel injection used in osteoarthritis care when symptoms persist and simpler measures have not been enough. In the US, care teams should confirm the current FDA-cleared or approved labeling and the latest instructions for use before stocking or administering it.
Why this matters operationally is straightforward. A single-visit option may reduce repeat appointment burden, but it also concentrates the key tasks into one encounter: confirming fit, reviewing precautions, documenting prior care, handling the product correctly, and giving clear discharge instructions. It is not a cure for osteoarthritis, and it should not be framed as a substitute for the broader management plan.
For format context, clinics comparing pack type and supply details can review the Monovisc Prefilled Syringe. Product-page review is only one part of the decision. The harder and more important work is matching the injection to the right clinical and administrative setting.
This briefing is written for licensed clinics and healthcare professionals.
How It Works and When It May Be Considered
Hyaluronan is a normal component of synovial fluid. In osteoarthritis, the joint environment may change in ways that reduce lubrication and shock absorption. Viscosupplementation aims to supplement that environment. At a high level, the goal is symptom management, not cartilage regrowth, and expectations should stay grounded in that distinction.
In practice, teams often consider this class when knee osteoarthritis symptoms continue despite conservative measures. That usually means the chart already reflects a diagnosis, symptom burden, prior noninvasive management, and the reason an injection pathway is being reviewed. Exact sequencing varies by clinician, facility, and payer. For that reason, selection should be policy-aware rather than brand-led.
A common mistake is treating any viscosupplement as a stand-alone fix. When load management, exercise-based care, weight strategy, bracing, analgesic review, or planned follow-up fall away, even an appropriately selected injection may appear to underperform. There is no single universal mistake that makes every painful knee worse, but immediate overloading of a symptomatic joint and weak follow-up planning are common avoidable problems.
Typical Selection Questions
- Confirmed diagnosis and side of treatment are clearly documented.
- Prior conservative care is listed in a way payers can follow.
- Past injection history and prior adverse reactions are reviewed.
- Active skin issues or infection risk near the site are assessed.
- Expectation setting is realistic and not framed as immediate or guaranteed relief.
Why it matters: A single-injection visit leaves less room to correct missed screening later.
Safety, Contraindications, and Monitoring Priorities
Safety review should start with the current instructions for use rather than class assumptions. Local post-injection reactions can occur with hyaluronan knee products, including pain, swelling, warmth, stiffness, or effusion at the treated joint. Many of these events are transient, but they still deserve clear documentation and follow-up instructions so routine post-procedure calls are easier to triage.
Care teams should also confirm contraindications and precautions before administration. In general, that means checking for active infection, skin disease or breakdown at the intended injection site, known hypersensitivity concerns related to the product or its components, and any presentation that suggests a different acute joint process may be underway. If the knee is unusually hot, markedly swollen, or clinically atypical, the right next step may be reassessment rather than routine injection flow.
Monitoring does not end when the syringe is empty. Staff need a consistent plan for what gets documented, what symptoms count as expected, and what should trigger earlier review. That is especially important when multiple clinicians or locations share the same aftercare queue.
When Follow-Up Should Accelerate
- Rapidly increasing swelling rather than mild expected soreness.
- Marked warmth or redness that continues to intensify.
- Fever, chills, or other systemic symptoms.
- New inability to bear weight or a sudden mechanical decline.
- Pain severity that seems out of proportion to a routine post-injection flare.
These features do not prove a serious complication on their own, but they do justify prompt clinical review to assess for infection, bleeding, crystalline arthritis, or another acute event. Clinics should decide in advance who receives these calls, how escalation is documented, and what same-day access looks like under local protocol.
Aftercare and Discharge Points to Standardize
After a Monovisc knee injection, clinics usually emphasize short-term activity moderation, symptom monitoring, and clear instructions on when to call back. The broad principle is simple: do not send patients back to strenuous, high-impact, or prolonged weight-bearing activity immediately without written guidance. Many instructions for use for this class advise avoiding strenuous activity or prolonged load on the joint for a short period after the injection, and clinics should align discharge wording with the current product instructions and local policy.
That answer is more useful than a vague do not overdo it message. Patients and front-desk teams need concrete language. If the discharge sheet is too loose, callbacks multiply and symptoms are harder to interpret. If it is too rigid, normal recovery questions become unnecessary alarm. Standardization helps both sides.
Care teams should also make it clear that there is no universal instant-response timeline. Some patients may notice little change early on, and some may have a short-lived flare before settling. The key operational point is not to promise speed or magnitude. Instead, document the baseline, give sensible activity and symptom advice, and define the follow-up path.
Minimum Discharge Elements
- Expected local soreness and what mild swelling may look like.
- Short-term activity limits based on the current instructions for use.
- How to handle routine comfort questions under clinic protocol.
- Red-flag symptoms that need same-day review.
- After-hours contact route and escalation backup.
- Planned follow-up timing and charting responsibility.
For many practices, the most useful discharge improvement is not a longer handout. It is a shorter, standardized one that the injector, nursing staff, and scheduling team all use the same way.
Coverage, Documentation, and Workflow
Coverage questions are common because viscosupplement products sit at the intersection of diagnosis, prior conservative management, plan policy, and interval rules. A Monovisc knee injection may be denied when the chart does not clearly show symptomatic knee osteoarthritis, prior conservative therapy, laterality, product-specific authorization steps, or plan-required timing for repeat treatment. Denials may also occur when the payer prefers a different product, limits site of service, or expects documentation that was discussed but never entered into the record.
That is why documentation needs to be built before the injection day. Useful records usually include the diagnosis and treated side, symptom history, conservative measures attempted, relevant imaging or exam context when required by policy, prior injection history, consent, and the rationale for the chosen product. After the encounter, the chart should also reflect the administered product details, lot and expiration tracking if applicable to your workflow, site, tolerance, discharge instructions, and follow-up plan.
Storage and handling deserve the same discipline. Follow the current label and instructions for use for receiving, storage, temperature expectations, and inspection before use. Do not assume all hyaluronan products share identical handling requirements just because they are in the same class.
Clinic Workflow Snapshot
- Verify diagnosis, laterality, and prior conservative care.
- Confirm payer rules, prior authorization status, and product preference.
- Review contraindications, site condition, and recent joint history.
- Order and receive stock under current storage and handling instructions.
- Document consent, procedure details, and administered product identifiers.
- Give written aftercare instructions with clear escalation language.
- Record follow-up responsibility for callbacks, outcomes, and adverse events.
Supply review should trace products to vetted distributors and verified channels.
Quick tip: Keep one standardized authorization packet for diagnosis, prior care, and product documentation.
Workflow consistency also helps when coverage is questioned later. If a payer asks why a claim was submitted, the record should answer that on its own. That means fewer missing pieces, fewer duplicate staff touches, and less back-end guesswork for the billing team.
How to Compare Other Hyaluronan Options
The main operational difference across viscosupplement products is often visit pattern rather than a simple better or worse label. Single-visit options can reduce repeat scheduling and repeated procedure notes. Series-based products may fit a different workflow, payer preference, or clinical pattern, but they usually require tighter scheduling discipline and more repeated documentation. Formulary status and plan preference often matter as much as brand familiarity.
Comparison should therefore start with logistics, policy, and consistency. If a clinic is choosing between products, helpful questions include how many visits the pathway creates, whether prior authorization is product specific, whether storage expectations differ, and how much repeat documentation staff can realistically support without leakage.
| Option Type | Examples | Operational Question |
|---|---|---|
| Single-visit options | Durolane 3 mL, Synvisc One | Will fewer injection visits reduce scheduling friction and missed follow-up steps? |
| Series-based options | Orthovisc, Euflexxa, Hyalgan, Supartz | Can staff support repeat appointments, repeat authorization steps, and consistent chart carry-forward? |
| Broader category review | Joint Injections | Which products align with local formulary, payer preference, and storage workflow? |
Compared with multi-visit series, a Monovisc knee injection can be easier to schedule when appointment friction is a real operational barrier. That does not make it automatically preferable. It means the best choice often depends on label fit, payer rules, clinic capacity, and how reliably the team can execute the full pathway from screening to follow-up.
Authoritative Sources
- FDA approval summary and labeling for Monovisc
- CMS billing and coverage article on knee hyaluronan
- AAOS guideline on non-arthroplasty knee osteoarthritis
Further Reading
For most clinics, the decision is straightforward when the indication is clear, the patient has already tried conservative care, and the workflow can support accurate documentation, handling, and follow-up. The harder part is consistency. Standardized screening, discharge advice, and payer documentation usually matter more than any single brand discussion.
If your team is reviewing knee injection pathways, use this topic as a checklist: confirm the label, confirm the policy, confirm the discharge process, and confirm the record can support the claim later. That approach keeps the discussion clinical, operational, and easier to audit.
This content is for informational purposes only and is not a substitute for professional medical advice.