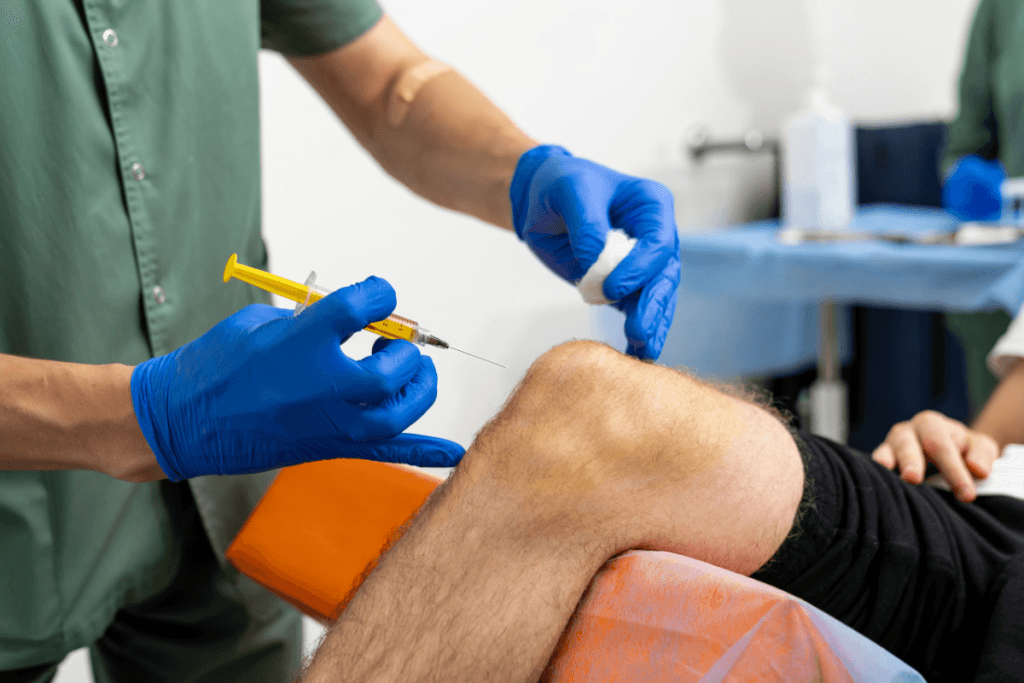
The main types of gel injections for knees are hyaluronic acid products used for viscosupplementation, meaning they supplement the lubricating properties of synovial fluid in the joint. Clinics usually classify them by labeled course length, formulation characteristics, packaging, sourcing requirements, and payer rules. That classification matters because it affects scheduling, consent language, post-injection triage, charting, inventory control, and coverage documentation.
This clinic-facing update keeps the focus on operations rather than brand promotion. Use it to align front desk scripting, clinical documentation, billing review, and procurement discussions. For broader product navigation, the Joint Injections category can serve as a browsable reference point for clinic teams.
Key Takeaways
- Gel injections usually mean intra-articular hyaluronic acid.
- Products differ by labeled course structure, formulation, and packaging.
- No single gel injection brand is universally best for every patient.
- Local pain, swelling, warmth, and stiffness are common counseling topics.
- Coverage review depends on diagnosis, laterality, prior care, and documentation.
How Clinics Classify Types of Gel Injections for Knees
Clinics can group types of gel injections for knees by how the product is used in a course, how the hyaluronic acid is formulated, and how the item fits the clinic workflow. This is more useful than starting with a brand list alone. A brand-only discussion can miss scheduling burden, payer preferences, lot tracking, and patient counseling needs.
Hyaluronic acid, often shortened to HA, is a naturally occurring component of synovial fluid. Intra-articular HA products are injected into the knee joint space. They are used for selected people with knee osteoarthritis, but they are not cartilage-regrowth therapies. They also differ from corticosteroid injections, which are used for anti-inflammatory effects in other clinical contexts.
Course length and scheduling
One practical distinction is course structure. Some HA products are labeled for a single-injection course. Others are supplied for multi-injection courses, often discussed in practice as a series. When referral notes mention a three-shot gel series, staff should confirm the exact product, labeled schedule, affected knee, and payer authorization terms before scheduling.
Course length affects more than appointment count. It changes inventory allocation, missed-visit risk, documentation repetition, and the number of post-procedure touchpoints. A clinic that stocks more than one HA option should define who can substitute products, how substitutions are approved, and how patients are notified when a plan changes.
Formulation and source terms
Another distinction involves formulation. Some HA products are described by molecular characteristics, cross-linking, or source. Some are avian-derived, while others are produced through non-animal processes. These details can matter for product selection, patient history review, and consent discussions, but staff should avoid making unsupported superiority claims.
Common knee gel injection brands that clinics may encounter include Synvisc, Euflexxa, Orthovisc, Monovisc, Durolane, Hyalgan, and Supartz. Product names should be documented exactly as supplied. If a team is reviewing a specific item record, a listing such as Supartz should be matched against the clinic formulary, product labeling, and internal purchasing controls.
Why it matters: Classification helps separate clinical choice from billing, inventory, and scheduling constraints.
Safety Counseling: Side Effects, Flares, and Escalation
Safety counseling should explain expected local reactions and define escalation steps before the patient leaves the clinic. Knee gel injections side effects commonly discussed in practice include injection-site pain, temporary swelling, warmth, stiffness, bruising, or a full feeling in the joint. These reactions are usually handled through the clinic protocol and the treating clinician’s instructions.
Use consistent language across the team. A front desk script should not diagnose by phone or promise a specific recovery pattern. It should capture the symptom, timing, affected knee, severity, fever status, and any functional change, then route the concern according to policy. Clinical notes should be more specific than a brief phrase such as tolerated well.
Red flags that need clinician triage
Marked swelling, severe or worsening pain, fever, drainage, spreading redness, or systemic symptoms need prompt clinician review. Clinics should define who receives these calls, how quickly they are assessed, and where the triage note lives in the record. This reduces inconsistent advice and supports quality review if a complication is later evaluated.
Patient-facing materials should also state that response varies. Some people ask why knee pain feels worse after a gel injection. A short-term flare can occur after intra-articular procedures, but worsening symptoms should still be routed through the clinic’s clinical pathway. Avoid reassurance that could delay assessment when symptoms fall outside the expected range.
Recovery and Activity Questions to Standardize
Recovery guidance works best when it is standardized but not personalized beyond the clinician’s instructions. Patients commonly ask about walking, driving, work, stairs, and exercise after knee gel injections. The safest clinic workflow is to give a written after-visit summary that reflects the medical director’s protocol, product labeling, and the specific procedure note.
For walking questions, staff can use protocol-based language rather than broad permission. Some patients may be allowed to walk normally after the visit, while others may be advised to limit activity for a short period. The answer depends on baseline function, the treated knee, pain level, assistive device use, and provider preference.
Driving questions need the same caution. The treated side, comfort with braking, baseline mobility, and any medications given during the visit can influence the recommendation. Exercise questions should be routed to the clinician’s plan, especially for patients returning to sport, heavy labor, or supervised rehabilitation.
An effective after-visit summary should include the treated knee, expected local symptoms, activity instructions, medication guidance if provided by the clinician, contact instructions, and escalation symptoms. It should also tell the patient what information to report if they call later, such as symptom onset, swelling pattern, fever, and functional change.
Brand Comparisons Without Overpromising
Brand comparison questions should be answered through defined decision factors, not broad claims about the best gel shot. Search terms such as Euflexxa vs Synvisc, Orthovisc vs Synvisc, Monovisc vs Synvisc, and Durolane knee injection reflect real patient interest. In clinic communication, those comparisons should stay anchored to labeling, payer rules, formulation details, prior response, patient history, and clinician judgment.
When a patient asks which product is most effective, a neutral answer is usually strongest. There is no universal winner across all patients and practice settings. A product that fits one clinic’s workflow may be less practical for another because of authorization rules, course structure, stocking limits, or provider preference.
Gel products versus corticosteroid injections
Gel injections and corticosteroid injections are not interchangeable categories. HA viscosupplementation is intended to supplement joint lubrication. Corticosteroids are anti-inflammatory medicines used in selected scenarios, often with different counseling, contraindication, timing, and payer considerations. Clinics should avoid presenting one category as automatically better than the other.
The practical comparison starts with the clinical question. Is the visit about osteoarthritis symptom management, an inflammatory flare, prior response, upcoming procedures, or payer step requirements? Then the team can document the rationale for the selected pathway without drifting into unsupported claims or patient-specific advice outside the treating clinician’s scope.
For practice managers, types of gel injections for knees also need to be compared against clinic capacity. Multi-injection courses require more appointment slots and follow-up tracking. Single-injection courses may simplify scheduling but still require the same attention to consent, lot capture, laterality, and payer rules.
Documentation, Coverage, and Cost Context
Coverage review should separate clinical appropriateness from benefits counseling. Patients may ask about knee gel injections cost or whether insurance covers a gel injection course. Staff can explain that coverage varies by plan, policy, diagnosis details, prior treatment history, and claim documentation. Patient-specific financial details should be handled by trained billing personnel.
From a charting standpoint, the recurring denial risk is missing or inconsistent documentation. Notes should show the osteoarthritis diagnosis, laterality, relevant history, functional limitation, prior conservative care when required, product used, procedure details, and follow-up plan. The level of detail should match clinic policy and payer requirements.
Checklist: Documentation elements to verify
- Diagnosis and laterality are clear.
- Symptoms and function are described.
- Prior therapies are documented when relevant.
- Product name is recorded accurately.
- Lot details are captured per policy.
- Procedure note is complete and signed.
- After-visit instructions are stored in the record.
Medicare and commercial payer policies can change. Use current payer policies, local coverage information when applicable, and the exact product record when preparing authorization or appeal materials. Avoid copying generic medical necessity language that does not match the visit note.
Sourcing, Traceability, and Inventory Workflow
Procurement controls are part of the clinical workflow for viscosupplementation products. HA injections are high-visibility items because patients ask about them, payers review them, and inventory errors can be costly. A consistent receiving process helps the clinic confirm product identity, lot number, expiry, storage requirements, and chain-of-custody records.
MedWholesaleSupplies serves licensed clinical accounts with brand-name medical products sourced through vetted distributor channels. For clinics planning around US distribution, the operational priority is still the same: verify supplier credentials, confirm product records, and store items according to labeling and site policy.
Stocking decisions should be made with input from clinical leadership, billing, and procurement. If the clinic uses more than one HA brand, define substitution rules before product is needed in the procedure room. If the product is patient-specific under a payer process, staff should know how it is labeled, stored, and reconciled before administration.
- Verify approved purchasers and clinic credentials.
- Confirm formulary choices and substitution rules.
- Procure through approved supplier channels.
- Reconcile received product to invoice and packing records.
- Store according to labeling and site policy.
- Document product, lot, site, laterality, and clinician.
- Retain records needed for audits and recalls.
Quick tip: Keep product inserts, lot records, and administration details easy to retrieve.
A consistent framework for types of gel injections for knees helps clinical, billing, and procurement teams speak the same language. The goal is not to force one product preference. It is to standardize definitions, counseling, documentation, and inventory controls so each case can be reviewed cleanly.
Authoritative Sources
When protocols, patient handouts, and payer notes are updated, use primary labeling for the exact item plus neutral professional guidance. These sources are useful starting points for broader policy review.
- AAOS OrthoInfo on viscosupplementation
- American College of Rheumatology osteoarthritis guidance
- CMS Medicare Coverage Database search
This content is for informational purposes only and is not a substitute for professional medical advice.