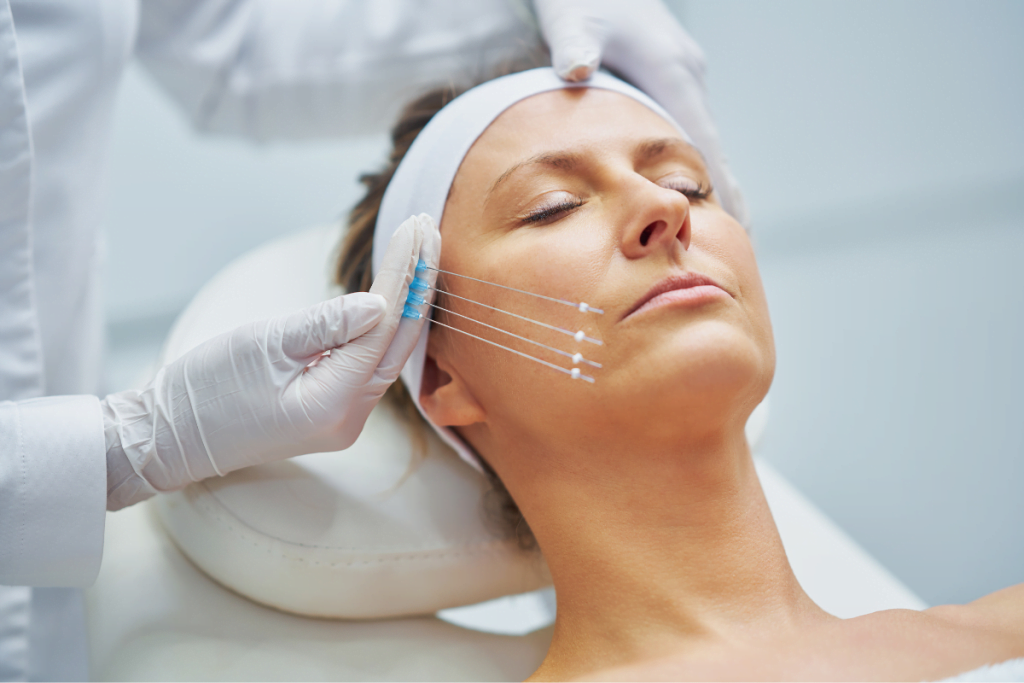
Disadvantages Of Thread Lift: Risks are best understood as planning risks, not just procedure risks. Thread lifts can provide modest, non-surgical soft-tissue repositioning, but they can also cause bruising, swelling, pain, puckering, asymmetry, visible threads, infection, and dissatisfaction. For licensed aesthetic teams, the main question is whether the patient, anatomy, consent process, technique, product documentation, and follow-up pathway justify the treatment.
Key Takeaways
- Expected effects include bruising, swelling, tenderness, tightness, and temporary contour change.
- Complications may include infection, hematoma, thread exposure, migration, persistent pain, and asymmetry.
- Results are usually subtle and temporary, so expectation-setting is a core safety step.
- Patient selection often determines whether thread lift disadvantages become predictable problems.
- Clinic checks should cover training, consent, sterility, product records, aftercare, and escalation.
What Thread Lifts Can and Cannot Reliably Do
A thread lift places absorbable or non-absorbable threads under the skin to reposition soft tissue. Some thread materials may also stimulate collagen remodeling as they absorb. The visible effect is generally more limited than surgery, which is why the procedure should not be framed as a facelift substitute.
Thread lift disadvantages often appear when the indication is weak. Heavy soft tissue, advanced laxity, poor skin quality, or surgical-level expectations can make a technically adequate result feel disappointing. The procedure may still have a role in selected cases, but the consultation should separate realistic lift from marketing language.
Clinics that need basic material context can review PDO Threads before comparing procedural risks. For broader thread-related education, the Threads Topic Hub can help teams organize deeper reading around treatment concepts and safety discussions.
Not all thread systems behave the same. Material, barb design, insertion plane, vector selection, and anchoring strategy can influence planning. When teams compare concepts such as Mint PDO Threads or Silhouette Soft, training, manufacturer instructions, local scope, and documentation standards should guide use.
Common Side Effects Versus Complications
Thread lift side effects usually involve short-term tissue response. Bruising, swelling, tenderness, entry-point discomfort, tightness, and mild surface irregularity can occur after tissue passage. These effects still need clear counseling, because patients may interpret normal recovery as a complication if expectations were vague.
Contour concerns are among the most visible problems. Puckering, dimpling, skin folding, or uneven lift may relate to thread depth, tissue tension, vector choice, edema, or anatomy. Some irregularity may soften as swelling changes. Persistent, worsening, painful, or skin-compromising distortion needs clinical review.
More serious thread lift complications can include infection, hematoma (localized blood collection), thread exposure, thread migration, persistent pain, visible or palpable threads, and significant asymmetry. Less common concerns can include nerve irritation, scarring, and vascular compromise, depending on the treatment area and technique. Consent should match the planned procedure rather than rely on generic wording.
| Concern | How Clinics Should Frame It | Escalation Signal |
|---|---|---|
| Bruising and swelling | Often expected after tissue passage | Rapid expansion, severe pain, or firmness |
| Puckering or dimpling | May reflect tension, depth, or settling | Persistent distortion or skin compromise |
| Asymmetry | Can reflect edema, vectors, or placement | Marked imbalance after the review window |
| Visible threads | Requires assessment of depth and position | Exposure, extrusion, irritation, or breakdown |
| Infection risk | Requires sterile technique and monitoring | Spreading redness, drainage, fever, or worsening pain |
| Hematoma | May follow vessel injury | Increasing swelling, discoloration, or pressure |
Why it matters: Early triage separates expected healing from problems that need timely review.
Cosmetic dissatisfaction also belongs in the risk discussion. A patient may have no infection, exposure, or hematoma and still feel the outcome failed. This is common when the expected change was described too strongly, before-and-after images were overinterpreted, or the patient’s laxity exceeded what threads could reasonably address.
Recovery, Downtime, and Settling Expectations
Thread lift recovery is often shorter than surgical lifting, but it is not always easy. Patients may report tightness, soreness, swelling, bruising, tenderness at entry points, and temporary changes in facial movement or surface contour. Clinics should avoid describing recovery as effortless.
Thread lift recovery time varies by thread type, area treated, tissue response, bruising, edema, aftercare adherence, and technique. Face threads may look tight or irregular at first, then settle over days to weeks. A clinic should not promise a fixed final appearance by a specific date, because tissue response is variable.
Aftercare instructions should be written, consistent, and aligned with the clinician’s protocol. Common themes include avoiding unnecessary manipulation of the treated area, following activity limits from the practice protocol, reporting worsening symptoms, and attending planned follow-up. Staff should not improvise different recovery advice across providers.
Visible threads after thread lift treatment, progressive pain, worsening swelling, drainage, fever, sudden contour change, or skin breakdown should trigger assessment rather than routine reassurance. A defined triage pathway helps reception staff, nurses, and clinicians use the same urgency language.
Patient Selection and Contraindication Review
Patient selection is one of the strongest safeguards against Disadvantages Of Thread Lift: Risks. The procedure may be a poor fit when laxity is advanced, tissue is heavy, expectations are dramatic, or the patient wants a long-lasting surgical degree of correction. In those cases, a non-surgical thread plan can create disappointment rather than value.
Screening should review active skin infection, inflammatory skin disease in the treatment area, impaired wound healing, bleeding risk, relevant medications, allergy history, prior aesthetic procedures, and previous adverse events. Medications that affect bleeding require clinical review. Patients should not be advised to stop prescribed therapy without appropriate oversight.
Some surgeons are cautious about thread lifts because results can be subtle, temporary, and technique-dependent. They may also consider whether prior threads could affect future surgical planes or tissue handling. That concern does not make every thread lift unsafe. It supports careful case selection and honest comparison with other options.
Consultation questions should identify the patient’s main concern, tolerance for downtime, willingness to accept temporary irregularity, scarring history, and understanding of alternatives. If the patient wants facial shape change, jawline refinement, fold correction, or skin-quality improvement, threads may need to be compared with other modalities instead of presented alone.
Clinic Safety Checks Before and After Treatment
Thread lift clinic safety checks turn general risk awareness into a repeatable workflow. Policies vary by jurisdiction and practice setting, so each clinic should align its process with local regulation, professional scope, supplier documentation, product instructions, and clinician training.
MedWholesaleSupplies serves licensed clinics and healthcare professionals through a B2B model. For product navigation, the Threads Product Category should be treated as a browseable product list, not a substitute for credentialing, hands-on training, or manufacturer-specific instructions.
Clinic Workflow Snapshot
- Verify scope: Confirm professional authority and training.
- Document screening: Record history, allergies, and contraindications.
- Check product records: Confirm sterility, lot details, and expiry.
- Standardize consent: Include limitations, alternatives, and complications.
- Prepare the field: Use aseptic technique and a procedural checklist.
- Record placement: Note thread type, area, pattern, and concerns.
- Give aftercare: Provide written instructions and escalation triggers.
- Plan review: Schedule follow-up and document patient reports.
Quick tip: Keep consultation language consistent across coordinators, clinicians, and follow-up staff.
Documentation should also capture expectation-setting. If a patient has borderline laxity or requests a surgical degree of change, the note should reflect that discussion. This protects continuity of care and helps future clinicians understand why a thread plan was accepted, modified, or declined.
Pros, Cons, and Alternatives in Treatment Planning
Thread lift pros and cons are clearer when the clinic separates lifting, volume, muscle movement, and skin quality. Threads are usually discussed for soft-tissue repositioning. They do not replace the roles of fillers, botulinum toxins, resurfacing, biostimulation, topical therapy, or surgery.
For expression lines and muscle-related movement, teams may compare thread-based lifting with neuromodulator planning through PDO Threads vs Botox. For volume loss or fold support, filler planning may be more relevant, and governance concepts from Dermal Filler Safety Protocols can support broader injection safety discussions.
Skin quality may need a different pathway. Texture, pigmentation, photodamage, fine crepiness, and acne scarring are not corrected by lifting alone. Depending on the clinical context, resurfacing, peels, topical regimens, or regenerative approaches may be more relevant than threads.
Before-and-after images should be used carefully. Photos can show possible change, but they cannot guarantee the same outcome. Lighting, expression, baseline anatomy, swelling, timing, and camera angle all affect interpretation. Clinics should explain that images are educational examples, not outcome promises.
When a Thread Lift Goes Wrong
A thread lift gone wrong can mean several different events. It may refer to dissatisfaction, persistent puckering, visible threads, infection, hematoma, migration, severe asymmetry, or pain that does not follow the expected recovery pattern. The first step is to define the concern clinically rather than respond only to the phrase.
Triage should consider severity, timing, progression, and associated symptoms. Stable bruising differs from expanding swelling. Mild tightness differs from escalating pain. A small contour irregularity differs from thread exposure, drainage, fever, or skin breakdown.
Management should stay within the clinician’s competence, training, and local regulation. When infection, significant bleeding, neurologic concern, severe pain, skin compromise, or uncertain anatomy is present, escalation is safer than delayed reassurance. Documentation should include photographs when appropriate, patient communication, assessment findings, and the plan.
For product-specific inventory review, individual thread listings such as Intraline Cog may help teams identify product names and categories. Procurement review should remain separate from clinical competency, consent, and complication-management decisions.
Authoritative Sources
- Review procedure risk framing from the American Society of Plastic Surgeons safety overview.
- Compare general recovery expectations with the Cleveland Clinic thread lift overview.
- Read complication detail in this PubMed facial thread lifting review.
Practical Recap for Licensed Clinics
A useful review of Disadvantages Of Thread Lift: Risks should leave clinics with three priorities: choose the right patient, document realistic consent, and prepare a clear follow-up plan. Threads can fit selected non-surgical aesthetic plans, but they require disciplined screening and careful explanation.
The strongest processes treat thread procedures as more than quick appointments. They include anatomy review, sterile technique, product verification, written aftercare, and escalation planning. That structure helps teams discuss thread lift risks without minimizing complications or overpromising results.
This content is for informational purposes only and is not a substitute for professional medical advice.