Key Takeaways
- Duration varies: Product, anatomy, and placement factors interact.
- “Settling” is multifactorial: Edema, product hydration, and tissue dynamics affect appearance.
- Risk and longevity are linked: Overcorrection and superficial placement can persist.
- Documentation matters: Standard photos and lot tracking support follow-up discussions.
Overview
Licensed clinics are frequently asked, how long does filler last under eyes, especially for tear trough (under-eye hollow) correction. A precise answer is rarely appropriate. Longevity depends on filler chemistry, injection plane, local lymphatic drainage, and patient-specific factors. The goal of this page is to help healthcare professionals frame duration expectations in clinical terms, while staying aligned with product labeling and local scope rules.
Under-eye augmentation typically uses hyaluronic acid (HA) filler (a water-binding gel volumizer). HA products are generally considered temporary. However, “temporary” does not mean predictable. In low-mobility zones, material can appear to persist longer than expected. In edema-prone patients, a small volume can look “present” for an extended period due to fluid shifts rather than persistent gel volume alone.
Why this matters: duration questions often sit beside concerns about dissatisfaction. You may hear phrases like “under eye filler gone wrong” or “under eye fillers ruined my face.” Those complaints can reflect contour irregularity, chronic swelling, blue-gray discoloration, or visible product. A duration conversation, done early, can reduce conflict later. For broader context on clinic workflows, see Facial Aesthetic Planning for assessment structure and recordkeeping rationale.
MedWholesaleSupplies operates as a B2B supplier for licensed clinics and healthcare professionals, so the emphasis here stays on clinic systems rather than consumer decision-making.
Core Concepts
When teams discuss how long does filler last under eyes, it helps to separate three concepts: material persistence, visible effect, and patient satisfaction. These can diverge. A small residual depot can remain without a desirable optical outcome, while edema can create an “overfilled” look even after product integration.
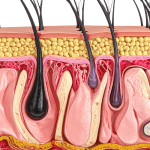
Anatomy and Optical Effects in the Tear Trough
The infraorbital region is unforgiving. Thin skin, minimal subcutaneous fat, and distinct retaining ligaments can make small contour changes look large. Depth also matters because superficial placement can create Tyndall effect (blue-gray discoloration) in lighter skin types. Conversely, deeper placement can reduce visibility but may not address skin texture or hyperpigmentation drivers of “dark circles.”
Plain-language translation helps during consults. Patients may describe “bags,” “shadows,” or “hollows.” Clinically, you may be balancing malar support, lid-cheek junction transition, and fluid dynamics. If midface volume loss is the primary issue, the under-eye result may be limited without adjacent support.
Product Variables: HA Rheology and Water Binding
HA fillers vary in concentration, crosslinking, and rheology (how a gel flows and resists deformation). These parameters influence lift, spread, and water attraction. A product with higher water binding may contribute to fullness that patients interpret as “still there,” even if the original intent was subtle blending.
Labels and instructions for use (IFU) should guide what a product is intended to do in specific planes. Avoid substituting general “filler duration” talking points for product-specific information. For a high-level refresher on categories and intended uses, Types Of Dermal Fillers provides a structured overview.
Placement Plane, Volume Strategy, and Tissue Response
Duration discussions should include technique-dependent variables without turning into procedural instruction. Under-eye contour is sensitive to small differences in depth, bolus size, and distribution pattern. Overcorrection can look persistent because the tissue cannot “hide” excess product. Superficial placement can remain visible even after partial degradation.
Instrument choice can also influence tissue trauma and bruising, which affects early appearance. Some clinics prefer microcannulas for certain passes, while others use fine needles based on training and anatomy. When teams are standardizing supply, examples include SoftFil Cannula for microcannula options and Fillmed Nanosoft Microneedles for fine-gauge access tools, depending on protocol and scope.
Patient Factors: Edema, Lymphatics, and Skin Quality
Under-eye tissue is prone to edema (swelling). Baseline festoons, malar edema (cheek swelling), allergic rhinitis patterns, or sleep-related fluid shifts can all exaggerate post-procedure fullness. In these cases, patients may report prolonged “puffiness” and interpret it as extended filler longevity.
Skin quality and dermal thickness also change what is visible. A small amount of product can show through thin skin, while thicker dermis may mask minor irregularities. Concurrent issues such as dermatitis or chronic irritation can complicate follow-up photos and symptom attribution.
Documentation: Photos, Baselines, and Language
“Under eye filler before and after” requests often come with expectations of dramatic transformation. In a clinic setting, “before and after pictures” function best as standardized documentation. Use consistent lighting, head position, and expression. Capturing “before and after smiling” can also be useful because dynamic contraction changes contour perception.
Tip: Consider adding a brief chart phrase differentiating “visible contour effect” from “material persistence.” That simple distinction can reduce confusion at follow-up.
How Long Does Filler Last Under Eyes: What Drives Duration
Longevity is best framed as a range of outcomes rather than a single timepoint. HA gels are gradually broken down and redistributed, but the visible result can change earlier or later than the material itself. In the under-eye, small changes in hydration and lymphatic drainage can shift appearance even when the product remains stable.
Patients also ask, “how long does under eye filler take to settle” and about “under-eye filler swelling stages.” A practical way to discuss this is to separate early post-procedure effects (bruising, transient swelling, and tissue remodeling) from later changes (gradual reduction in correction). When patients ask about “under eye filler recovery time,” set expectations around variability and follow-up checkpoints, rather than promising a fixed timeline.
It also helps to address the myth of “permanent under-eye filler.” Some materials can be long-lasting, but permanence is not a simple benefit in a high-risk aesthetic zone. A persistent contour issue can be harder to manage than a temporary one.
Practical Guidance
Duration questions often surface alongside cost, photos, and fear of complications. Patients may mention “under eye filler cost” or bring screenshots from social forums. Keep the conversation anchored to your clinic’s documented process, product labeling, and your informed-consent framework. For a risk-oriented refresher, Safety-First Protocols outlines clinic-level safety concepts that support consistent counseling.
To keep teams aligned, a short internal checklist can help standardize how you answer how long does filler last under eyes across providers and coordinators. That consistency reduces mixed messages, especially when different staff handle intake calls and follow-up messages.
Clinic Workflow Checklist for Duration and Follow-Up
Use this as a non-prescriptive workflow aid. Adapt it to your jurisdiction, training, and product IFU.
- Baseline capture: Standardized photos at rest and mild smile, with consistent lighting.
- Expectation framing: Document whether the goal is shadow reduction, contour blending, or both.
- Early change education: Explain that swelling can mimic overcorrection initially.
- Red-flag language: Provide clinic-specific instructions for urgent symptoms per protocol.
- Follow-up plan: Set a routine reassessment point, then adjust based on findings.
If a patient asks about “how many syringes for under-eye filler,” treat it as a clinical planning question, not a shopping metric. Volume depends on anatomy, adjacent support needs, and how much correction is appropriate for tissue tolerance.
For post-visit communication consistency, Post-Treatment Care Essentials can support your standard instruction templates without relying on informal online guidance.
Compare & Related Topics
Under-eye HA correction is often compared with midface augmentation, neuromodulators, and skin-quality treatments. The comparison is useful because patients may interpret “it didn’t last” when the real issue is that the dominant cause of shadowing was not volume loss. In other cases, a subtle under-eye correction can appear to last longer than expected because the under-eye is relatively low motion compared with perioral areas.
When discussing how long does filler last under eyes, it can help to contrast “duration of visible effect” with “duration of dissatisfaction risk.” An irregularity, a superficial hue change, or a swollen pocket under eyes after filler treatment can remain noticeable even if the product is slowly diminishing. That is why prevention, conservative planning, and documentation matter more here than in many other facial zones.
If questions drift toward corrective pathways, keep references neutral and policy-based. A clinic may discuss evaluation and potential reversal options within scope and training. For background reading, Dermal Filler Removal Options summarizes considerations that often come up after dissatisfaction. For myth-busting language that helps front-desk teams respond consistently, see Dermal Filler Myths.
Role clarity also supports safer triage. If your clinic uses a team-based model, Clinic Team Roles is a useful internal reference for aligning tasks to credentials and supervision requirements.
Clinic Ordering and Compliance Notes
Supply chain choices affect documentation quality and risk management. Clinics typically need reliable lot tracking, documented sourcing, and consistent ancillary supplies. MedWholesaleSupplies provides brand-name medical products through vetted distributors and verified supply channels, which supports audit-ready purchasing records when your compliance team requests them.
Ordering on MedWholesaleSupplies is restricted to licensed clinics and healthcare professionals. Keep onboarding documents current, and ensure ordering access aligns with your medical director’s policies.
For teams standardizing procurement, the Dermal Fillers Category page can be used as a reference hub for assortment planning, while Dermal Fillers Resources is helpful when you want related education in one place. If your protocols specify microcannula lengths and gauges, Softfil Precision Micro Cannula 25G 50mm is an example listing you can map to your internal preference cards.
Why this matters operationally: when patients return with “under eye filler before and after” concerns or report “under-eye fillers side effects long-term,” your ability to reference product identifiers, placement notes, and photo baselines can make follow-up more efficient and less subjective.
Authoritative Sources
Use regulator and specialty-society resources to keep counseling language aligned with current safety communications. This is especially important when patients arrive with social-media narratives like “under eye filler cost reddit” or “under eye filler before and after reddit,” which often mix anecdote with incomplete clinical context.
- FDA overview of dermal fillers and risks (device category background and safety framing).
- American Academy of Dermatology overview of soft tissue fillers (general considerations and adverse event awareness).
Recap: how long does filler last under eyes is a practical question, but it is best answered through a structured lens. Separate product persistence from visible effect, account for edema and optical factors, and rely on consistent documentation. When your team uses shared language and standardized records, duration discussions become clearer and more defensible.
This content is for informational purposes only and is not a substitute for professional medical advice.