Key Takeaways
Clinicians often ask, what are the layers of the epidermis, when reviewing barrier risks and procedure depth. This overview keeps the anatomy practical for documentation, education, and product selection in clinic workflows.
- Five-layer model: Thick skin includes stratum lucidum between granulosum and corneum.
- Thin vs thick skin: Most body sites have four layers, not five.
- Barrier logic: Corneocytes and lipids drive permeability and irritation risk.
- Depth matters: Many techniques target the dermis, not epidermis.
- Terminology consistency: Use “stratum basale” and a plain-language gloss once.
Overview: What Are The Layers Of The Epidermis
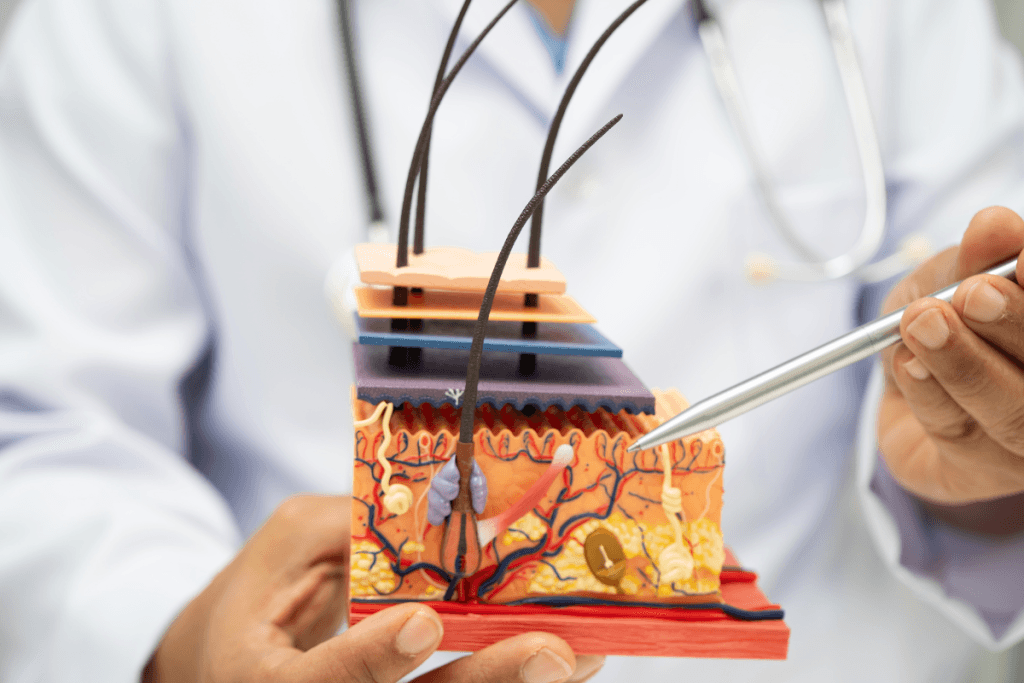
The epidermis is the outer skin layer that provides a protective interface with the environment. It is a stratified squamous epithelium made mostly of keratinocytes (skin-forming cells). Clinically, it supports barrier function, hydration control, and antimicrobial defense. It also influences visible texture and pigment patterns. Small differences in thickness can change how skin responds to friction, adhesives, and energy-based devices.
This article summarizes the layers, their order, and their core functions. It also connects epidermis anatomy to the dermis and hypodermis (subcutaneous layer) for depth-aware documentation. MedWholesaleSupplies operates as a B2B supplier model for healthcare professionals, which means content is written for clinic teams, not consumers.
Core Concepts
When you map epidermis function to clinical decisions, start with structure. The epidermis lacks blood vessels, so it depends on the diffusion of nutrients and oxygen from the dermis. That constraint explains many normal patterns, including surface desquamation and sensitivity to ischemia. In practice, clear naming helps reduce ambiguity in notes, consent language, and procedure planning.
MedWholesaleSupplies focuses on brand-name medical products for licensed practices, so teams often pair anatomy refreshers with formulary reviews. You can also use this section to align how staff describe “surface skin” versus deeper tissue planes.
Epidermis Anatomy, Cells, and Turnover
The epidermis is organized into layers that reflect keratinocyte differentiation from basal proliferation to surface shedding. Melanocytes (pigment-producing cells) primarily reside in the basal layer and transfer melanin to keratinocytes. Langerhans cells (antigen-presenting immune cells) are mainly located in the stratum spinosum and support cutaneous immune surveillance. Merkel cells contribute to touch sensation, especially in specialized skin.
Turnover timing varies by age, site, and inflammation, but the directional concept is stable. Cells originate near the basement membrane zone, migrate upward, and eventually form an anucleate surface barrier. This model helps explain why many superficial changes present first as stratum corneum findings, while deeper inflammatory patterns involve dermal vasculature and appendages.
Layers of Epidermis in Order (Thin vs Thick Skin)
Most teaching uses the “layers of epidermis in order” framework. In thin skin, you commonly describe four layers: stratum basale, stratum spinosum, stratum granulosum, and stratum corneum. Thick skin adds a fifth layer, stratum lucidum, classically in palms and soles. The “5 layers of epidermis” phrasing is accurate for acral thick skin, but it can mislead if applied globally.
Note: If a chart template defaults to five layers, add a brief footnote that most sites lack a distinct lucidum.
The table below summarizes what teams usually document, along with plain-language cues that can help trainees.
| Layer | Plain-language synonym | Key features | Why it can matter in clinics |
|---|---|---|---|
| Stratum basale | Growth layer | Mitotic keratinocytes; melanocytes; basement membrane attachment | Reference point for epidermal regeneration and pigment distribution |
| Stratum spinosum | “Spiny” cell layer | Desmosomes; early keratin bundling; immune surveillance | Common site of eczematous change on histology |
| Stratum granulosum | Granule layer | Keratohyalin granules; lamellar lipid release; tight barrier assembly | Explains barrier compromise and irritant penetration patterns |
| Stratum lucidum | Clear layer (thick skin) | Compact, translucent zone in thick skin | Context for acral friction tolerance and callus formation |
| Stratum corneum | Outer dead-cell layer | Corneocytes + lipid matrix; desquamation; water retention | Primary determinant of topical permeability and tape/adhesive interactions |
Layer-by-Layer Functions: Basale to Corneum
Stratum basale anchors the epidermis to the dermis through the basement membrane zone. It houses proliferative keratinocytes and supports continual renewal. When you describe superficial erosions, it helps to specify whether the basal layer is likely intact, since re-epithelialization depends on remaining basal and adnexal reservoirs.
Stratum spinosum follows, where cells develop prominent intercellular bridges from desmosomes. These junctions improve mechanical cohesion between keratinocytes. When clinicians use “spongiosis” in dermatopathology summaries, they often refer to edema that separates these connections, producing characteristic microscopic spacing and clinical oozing or vesiculation.
Stratum granulosum marks a key shift toward barrier creation. Cells accumulate keratohyalin granules and participate in lipid processing. This is where lamellar bodies contribute to the extracellular lipid matrix that later supports stratum corneum integrity. In plain terms, it helps “seal” the surface, which is why disruption here can increase irritant sensitivity.
Stratum lucidum location is typically limited to thick skin, especially palms and soles. Its stratum lucidum function is often described as added protection in high-friction areas. In charts, many teams simply note it as a thick-skin feature rather than a universally present layer.
Stratum corneum completes the barrier with flattened corneocytes embedded in lipids. This “brick-and-mortar” organization explains why dehydration, over-exfoliation, or contact dermatitis often presents first as scaling, roughness, and increased transepidermal water loss. These observations also frame why pre-procedure prep can change surface feel without changing deeper tissue planes.
Connecting Epidermis, Dermis, and Hypodermis
Many clinical misunderstandings come from mixing the epidermis with the dermis and hypodermis. The dermis is a connective tissue layer with blood vessels, nerves, and collagen-elastin architecture. Clinicians often divide it into the papillary layer of dermis (superficial, looser connective tissue) and the reticular layer of dermis (deeper, denser collagen). This “structure of dermis” framework supports discussion of tensile strength, wound remodeling, and scar behavior.
The hypodermis, also called the subcutaneous layer, sits beneath the dermis and contains adipose tissue and fibrous septae. It affects contour, insulation, and mechanical cushioning. When teams document depth, it can help to specify “epidermal,” “dermal,” or “subcutaneous” rather than using vague terms like “superficial” alone.
MedWholesaleSupplies sources inventory through vetted distributor networks, which supports consistent lot documentation when clinics standardize supplies across procedures. That operational discipline pairs well with standardized anatomical terms in charting and training.
Practical Guidance
In day-to-day clinic work, clarity beats memorization. The goal is consistent language across staff, especially when you explain why a finding is epidermal versus dermal. A simple approach is to document the visible surface change, then add a likely layer “home” only when it supports the plan of care. You can also tie education materials to a single diagram set so staff use the same labels.
If your team is building a short in-service around what are the layers of the epidermis, keep it anchored to workflow touchpoints. Start with “layers of epidermis labeled” diagrams, then link each layer to one observable feature. The Clinical Skincare hub can help align terminology when protocols mention cleansers, occlusives, or barrier-support products.
Documentation checklist for skin findings
Use a consistent template so notes stay comparable over time. Keep the writing descriptive and avoid implying histology when you did not sample tissue.
- Site and laterality: Include body site and exposure patterns.
- Surface description: Scale, fissure, vesicle, crust, erosion.
- Color changes: Erythema, hyperpigmentation, hypopigmentation.
- Depth language: Epidermal change versus dermal swelling versus subcutaneous nodularity.
- Barrier context: Hydrated, xerotic, macerated, or occluded.
Procedure-depth communication (without overpromising)
Patients often use “skin” as a single compartment. Staff can reduce confusion by pairing a clinical term with a plain-language synonym once, then staying consistent. For example, “epidermis (outer skin layer)” versus “dermis (support layer).” This small change can reduce miscommunication about expected surface changes versus deeper tissue effects.
When clinics discuss needling, abrasion, or surface resurfacing, the key operational question is depth control and aftercare documentation. Tools and consumables vary, so teams often cross-reference device instructions and consumable specifications. For example, some clinics use Micronjet as a microneedle-based option when mapping superficial delivery workflows, while others reference Fillmed Nanosoft Microneedles for fine intradermal technique training.
MedWholesaleSupplies serves licensed clinics rather than direct-to-consumer buyers, which fits how most practices handle supply control and competency tracking. Keep competency checklists separate from marketing language, and anchor them to anatomy and device labeling.
Common pitfalls staff should avoid
Several patterns show up in audits and training reviews. They are easy to fix with a shared reference sheet.
- Overusing “five layers”: Most sites have no distinct lucidum.
- Calling all redness “epidermal”: Vascular responses live in the dermis.
- Confusing barrier with thickness: Barrier quality can vary without visible thickening.
- Assuming product effect depth: Many topicals primarily interact with the stratum corneum.
When protocols mention moisturizers or occlusives, keep the description structural. You can reference a representative clinic product like Zo Skin Hydrating Cream to anchor training language around surface hydration and corneum support, without implying a clinical outcome. If you also stock post-procedure masks, a similar neutral example is Jalupro Biocellulose Face Masks for illustrating occlusion and comfort steps.
Compare & Related Topics
Clinicians often learn the “3 layers of skin” model first: epidermis, dermis, and hypodermis. That framing works well for most clinic conversations. The “7 layers of skin” phrasing usually reflects subdividing the epidermis and dermis into more granular strata, or counting functional subzones. If you use that expanded model, define it in your materials so it stays consistent across staff.
To compare the layers of dermis and epidermis, focus on what each layer contains. The epidermis is cellular and avascular. The dermis contains vessels, nerves, adnexal structures, and collagen. The hypodermis adds fat lobules and fibrous septae. This is why edema and bruising patterns often map to dermal and subcutaneous tissue more than to epidermal compartments.
When teams revisit what are the layers of the epidermis, it can also help to contrast skin with other layered tissues. Joint injections, for example, require a different depth logic than skin procedures. If your clinic also trains on viscosupplementation counseling, you may find it useful to cross-reference Types Of Gel Injections for terminology alignment, Supartz Vs Euflexxa for product-class comparisons, or Hymovis Injection for counseling structure.
MedWholesaleSupplies uses verified supply channels to support clinic-grade sourcing. That sourcing model matters whenever your policies require traceability, whether the supply is for skin or musculoskeletal workflows.
Clinic Ordering and Compliance Notes
Ordering is restricted to licensed clinics and qualified healthcare professionals. In practice, this usually means your account setup should match facility licensing, authorized purchaser roles, and any prescriber identifiers required for regulated items. Keep internal policies for receiving, inventory counts, and product segregation aligned with your accrediting body and local regulations.
For teams who standardize education around what are the layers of the epidermis, compliance details still matter. Products used around the skin barrier can include topicals, devices, and prescription-only items, each with different documentation expectations. MedWholesaleSupplies supplies clinics through a B2B channel, and products are obtained via vetted distribution partners, which supports routine lot tracking and quality documentation. Storage and handling should follow the manufacturer label and your clinic SOPs, especially for items with specific environmental requirements.
Authoritative Sources
For deeper reference, use sources that separate gross anatomy, histology, and barrier physiology. The following links provide stable terminology and diagrams suitable for staff education.
MedWholesaleSupplies is designed for licensed clinics and healthcare professionals, so content emphasizes clear definitions and documentation-ready language. If you revisit what are the layers of the epidermis during onboarding, consider pairing a labeled diagram with one table that distinguishes epidermis, dermis, and hypodermis responsibilities. That approach reduces miscommunication across roles and supports consistent chart language.
This content is for informational purposes only and is not a substitute for professional medical advice.