Key Takeaways
This page reviews side effects of calcium infusion in monitored clinical settings. It focuses on recognition, documentation, and administration safety for licensed teams.
- Expect predictable reactions: flushing, nausea, and local IV discomfort are common.
- Watch for rate-related effects: hypotension (low blood pressure) and rhythm changes can occur.
- Protect the IV site: extravasation (leak into tissue) can cause significant injury.
- Use label-first protocols: dilution, line choice, and monitoring follow the product monograph.
- Document clearly: indication, baseline status, and response support continuity of care.
Overview
Intravenous calcium is used in several acute-care and peri-procedural contexts, most often as calcium gluconate injection. Because calcium is a high-impact electrolyte supplement, infusion technique and monitoring matter as much as drug selection. Teams should be familiar with expected reactions, rarer but higher-risk events, and the workflow steps that reduce preventable harm.
This article summarizes how infusion reactions can present, what factors increase risk, and what to capture in nursing and provider documentation. It also clarifies common terminology, including calcium gluconate IV administration, calcium gluconate indication language, and where calcium gluconate contraindications typically apply. MedWholesaleSupplies serves licensed clinics and healthcare professionals, so the lens here is clinical-trade workflow rather than patient self-management.
Note: Institutional policies vary. Use your facility’s protocols and the specific product monograph for calcium gluconate vial selection, preparation, and monitoring requirements.
Side Effects of Calcium Infusion: Recognition and Response
Clinicians usually categorize reactions into three groups: expected transient symptoms, infusion-site complications, and cardiopulmonary events. Many events are influenced by concentration, venous access quality, and administration rate. A structured assessment helps teams avoid anchoring on a single cause, especially in unstable patients.
In practice, symptom timing is informative. Immediate warmth or flushing may align with vasodilation (blood vessel widening). Local burning along the vein may suggest irritation or early phlebitis. New dizziness, chest discomfort, or palpitations should trigger broader evaluation, including ECG monitoring when indicated by protocol. When documentation is specific, downstream teams can distinguish a predictable reaction from a true adverse event.
Core Concepts
Common Indications and Formulations (Calcium Gluconate Focus)
IV calcium is used for defined indications such as hypocalcemia (low blood calcium) and for membrane stabilization in select toxicologic or electrolyte scenarios, per institutional protocols. In many facilities, calcium gluconate injection is the preferred formulation for peripheral administration because it is generally less irritating to veins than more concentrated calcium salts. Formulation choice affects line selection, dilution needs, and monitoring intensity.
Use consistent terminology in orders and notes. “Calcium gluconate uses” is a broad phrase, but clinical records should specify the intended physiologic goal (for example, correction of symptomatic hypocalcemia) and relevant baseline data. Clear indication language also helps interpret symptoms that occur during administration.
Mechanism of Action and Why Rapid Changes Matter
Calcium gluconate mechanism of action is best described as electrolyte repletion plus physiologic stabilization. Calcium participates in neuromuscular conduction and myocardial function. Rapid shifts can alter vascular tone and cardiac conduction, which is why monitoring and administration controls are commonly emphasized in calcium gluconate infusion protocol documents.
When teams see bradycardia (slow heart rate) or hypotension during infusion, the cause may be multifactorial. Rate, patient volume status, and concurrent medications can all contribute. Linking the event to timing and infusion parameters supports safer future care than documenting “reaction” alone.
Administration Factors That Drive Adverse Events
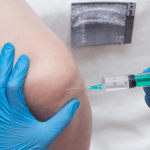
Many preventable complications relate to technique rather than the ingredient itself. Calcium gluconate IV administration typically requires attention to dilution, compatibility, and venous access. Peripheral lines that are small, positional, or placed in flexion zones increase the chance of infiltration and patient-reported burning. Infusion pumps and standardized concentrations reduce variation, especially when multiple staff members share the task.
Preparation steps also matter. “How to give calcium gluconate” should not be treated as a quick skill check. It is a sequence: confirm the order, verify labs and clinical indication, select the line, prepare and label the solution, and monitor to a defined endpoint. Align each step with local policy and the manufacturer’s instructions.
Adverse Effects: A Practical Classification
Calcium gluconate side effects can be framed as systemic versus local. Systemic reactions include warmth, flushing, nausea, headache, and a transient metallic taste, though patient reports vary. More serious systemic issues can include hypotension and arrhythmias, particularly when administration is rapid or when underlying cardiac disease is present. Local reactions include pain at the IV site, venous irritation, and phlebitis.
The table below is a documentation aid, not a diagnostic tool. It can help teams chart what happened and what was assessed.
| Observation | Common contributors | What to document |
|---|---|---|
| Flushing or warmth | Rate-related vasodilation | Onset time, infusion rate, vitals trend |
| Nausea or discomfort | Transient systemic effect | Severity, associated symptoms, interventions used |
| IV site burning | Irritation, small vein, concentration | Line location, patency checks, patient reports |
| Swelling or blanching | Infiltration/extravasation risk | Site exam, actions taken, escalation pathway |
| Rhythm changes | Rate, comorbid disease, interactions | ECG findings, timing, provider notified |
Contraindications, Interactions, and Special Contexts
Calcium gluconate contraindications commonly include hypercalcemia (high blood calcium) and clinical scenarios where IV calcium may increase risk. Interactions are also relevant. For example, caution is often highlighted with digoxin and other agents that affect conduction. Compatibility with IV solutions and co-infused drugs is another safety axis, especially in busy treatment bays.
Special populations require extra clarity in documentation. Pediatric protocols, pregnancy considerations, and renal impairment may change monitoring intensity and endpoint definitions. If your service uses calcium gluconate IV dose pediatric references, keep them in protocol form with version control. That approach prevents informal dosing drift and supports auditability.
Practical Guidance
Use a consistent checklist approach for preparation and monitoring. Calcium infusion events are easier to prevent when roles are clear and the workflow is standardized. This is especially true when the infusion is given during emergencies or high-throughput clinic sessions.
Below is a practical sequence aligned with typical calcium gluconate nursing responsibilities. It is intentionally label-forward, since calcium gluconate dose and rate details depend on the exact product monograph and the clinical context.
- Confirm the order context: indication, recent labs, and any ECG concerns.
- Screen for risk factors: baseline hypotension, conduction disease, and known hypercalcemia history.
- Choose venous access carefully: assess patency and avoid questionable peripheral sites.
- Prepare per monograph: follow calcium gluconate IV administration dilution instructions exactly.
- Monitor during administration: vitals trend, symptoms, and IV site assessment at defined intervals.
- Document objectively: timing, infusion parameters, observations, and escalation steps.
When documenting side effects of calcium infusion, avoid vague terms like “intolerant.” Instead, chart what occurred, what was assessed, and who was notified. If an IV-site issue is suspected, describe appearance, patient-reported pain, and line function checks.
For teams that also perform office-based injectables, it can help to standardize the safety mindset across workflows. The Injection Safety category is a useful internal hub for sharps and handling policies that support consistent practice.
MedWholesaleSupplies focuses on brand-name medical products for professional use, which is why traceability and documentation standards are emphasized across ordering and administration workflows.
Compare & Related Topics
Clinicians often need to distinguish infusion reactions from local tissue injury and from unrelated clinical deterioration. A few comparisons help sharpen the assessment.
Calcium gluconate vs calcium chloride: both provide calcium, but they differ in concentration and local irritation potential. Many protocols reserve more irritating formulations for specific settings and line types. If your team references “calcium gluconate classification,” keep it consistent as an electrolyte supplement, while documenting the exact salt and concentration used.
Infusion vs oral supplementation: calcium gluconate tablets are used for supplementation, while IV therapy is used for monitored correction or stabilization. Calcium gluconate tablets side effects often trend toward gastrointestinal intolerance rather than IV-site complications. Avoid conflating these in adverse event reporting, since the risk controls differ.
Infusion safety vs injection safety: dermal filler injections and IV infusions are distinct procedures, but both depend on aseptic technique, device integrity, and clear escalation pathways. For clinics that also provide aesthetic injectables, Safety First Key Protocols offers a complementary view of standardized safety steps across injectable services.
When reviewing side effects of calcium infusion in incident meetings, teams often benefit from using a common language for preventability. The post Wholesale Fillers Sourcing Standards is also relevant as a reminder that sourcing controls and documentation reduce downstream clinical uncertainty.
Clinic Ordering and Compliance Notes
Ordering and handling policies are part of medication safety. A reliable chain of documentation supports clinical decision-making when a reaction occurs, especially if multiple lots or presentations are in circulation. Clinics should also separate medication procurement workflows from device procurement workflows to prevent substitution errors.
Ordering through MedWholesaleSupplies is restricted to licensed clinics and qualified healthcare professionals. Keep internal records that tie the received product to the storage location, lot details, and the service line that uses it. MedWholesaleSupplies sources products through vetted distributors and verified supply channels, which supports traceability expectations in professional settings.
Storage and handling should follow the manufacturer’s labeling, including any light protection or temperature range statements. Use a receiving checklist that includes visual inspection, expiration verification, and reconciliation against the packing document. If your clinic stocks both infusion-related items and office injectables, consider separate binning and labeling conventions.
Tip: If your practice also orders injectables and devices, standardize your receiving workflow. The article How To Buy Cannulas outlines documentation habits that transfer well to medication receiving and inventory control.
For clinics that stock aesthetic cannulas and micro-needling devices, keep product selection clearly scoped to procedure type. For example, SoftFil Cannula and Fillmed Nanosoft Microneedles relate to subdermal techniques, not IV administration, but the same traceability and sterility checks apply.
Authoritative Sources
For prescribing, preparation, and monitoring specifics, defer to official labeling and institutional protocols. The sources below can support policy writing and staff education.
- DailyMed calcium gluconate injection labeling for monograph-based preparation and safety language.
- ISMP high-alert medication resources for broader medication safety framework and risk controls.
In summary, side effects of calcium infusion are best managed with structured monitoring, careful IV-site assessment, and label-aligned preparation steps. Strong documentation closes the loop across shifts and settings.
This content is for informational purposes only and is not a substitute for professional medical advice.