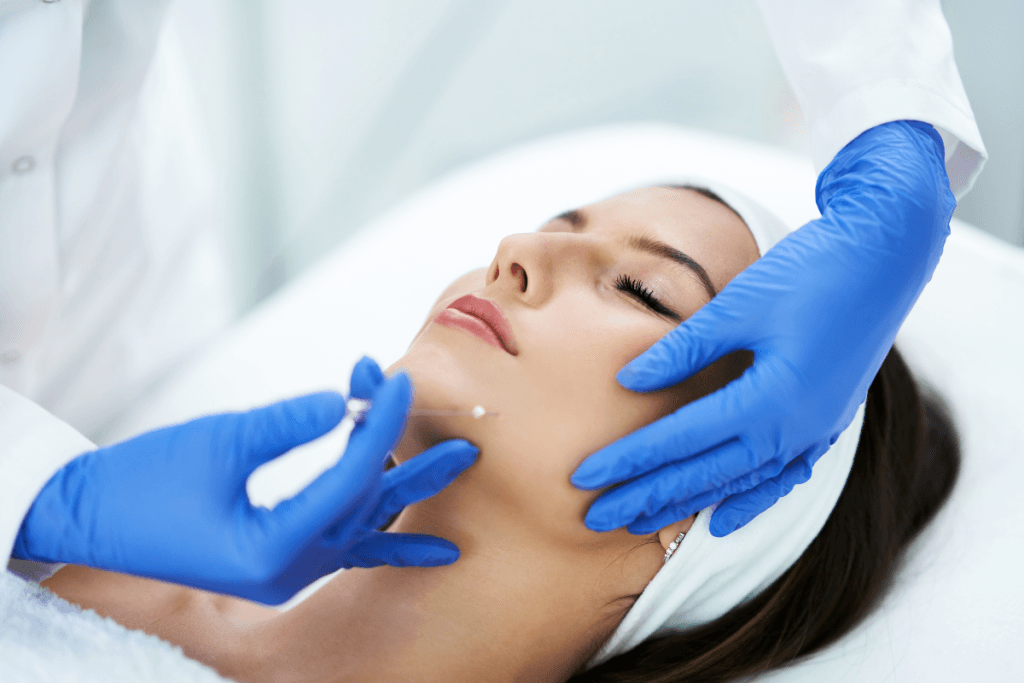
Mint PDO Threads for Clinics: Practical Workflow Guide is best understood as a clinic-facing framework for patient selection, planning, consent, traceability, and follow-up. It matters because thread outcomes are shaped as much by assessment and documentation as by placement itself. A safe program usually starts with trained providers, anatomy-led vector planning, label-specific instructions, standardized photography, written aftercare, and a clear escalation pathway.
This is not a substitute for hands-on training or the manufacturer’s instructions for use. For most practices, the real operational question is where thread lifting fits in the service line, which patients may be appropriate, and how the clinic will manage records, recovery, and complications before the first case is booked.
MedWholesaleSupplies serves licensed clinics and healthcare professionals.
Key Takeaways
- Screen candidacy before discussing thread counts or patterns.
- Use anatomy, skin quality, and laxity to set realistic goals.
- Keep consent, photography, lot tracking, and follow-up standardized.
- Review label-specific instructions and escalation plans before treatment day.
- Document prior threads for any later surgical or revision planning.
Using Mint PDO Threads in Clinical Workflow
Mint PDO threads are typically positioned as a minimally invasive option for lift and contour in selected patients. PDO means polydioxanone, an absorbable suture material. In clinic workflow terms, that makes thread lifting a combined device, anatomy, and documentation process rather than a simple add-on cosmetic service.
The key question is not only whether a patient wants more lift. It is whether the degree and pattern of tissue descent can be addressed predictably without surgery, whether the clinic has the right training and governance, and whether the expected result matches what a thread-based approach can realistically deliver.
Criticism of PDO threads usually comes from poor selection, overpromised results, weak follow-up, or attempts to use threads where surgery would be the more appropriate discussion. Mild to moderate laxity, clear goals, and careful planning are different from trying to replace a facelift in patients with heavy tissue descent or marked skin excess.
For broader context, clinics can browse the Threads Hub for related reading and compare device listings in the Threads Product Category when procurement teams review options.
Patient Selection, Consultation, and Contraindications
Good candidates are usually defined by anatomy and expectations first. In practice, the strongest consultations assess skin quality, tissue thickness, vector feasibility, asymmetry, prior procedures, scarring history, and the gap between requested lift and what threads may reasonably achieve.
What to cover in the first consultation
Start with the patient’s main concern in plain language, then translate it into exam findings. That may include jowl descent, midface ptosis (drooping), early jawline blunting, lower-face laxity, or contour asymmetry. Standardized photographs, facial movement assessment, and review of prior fillers, surgery, energy devices, or earlier thread placements help define whether a PDO thread lift fits the case.
Consent should be specific. It should cover likely short-term effects such as edema (swelling), ecchymosis (bruising), tenderness, temporary irregularity, asymmetry, palpable threads, skin puckering, or the need for reassessment. It should also explain that mechanical lift is not the same as surgical repositioning, and that visible improvement and durability can vary with tissue quality, facial movement, and the exact technique used.
When to defer or reconsider
Common reasons to defer can include active infection, inflamed acne or dermatitis in the treatment area, poor wound-healing history, unstable medical issues, unrealistic expectations, or anatomy that would make vector support unreliable. Anticoagulant use, recent dental or facial infection, recent procedures, and autoimmune history may also require closer review under clinic policy and the product’s official instructions.
Whether an RN can perform PDO thread procedures depends on state law, credentialing rules, training, supervising clinician requirements, and employer policy. A clinic should confirm scope of practice locally before scheduling cases, not after consent is signed.
Why it matters: Most avoidable thread-lift problems start with candidacy and expectations, not with the insertion step.
For teams building intake protocols, the Clinic Operations hub and the Mint PDO Threads tag can help standardize how consultations are documented across providers.
Planning the Case Before the Procedure Room
Safe planning starts before skin marking. A strong pre-procedure plan defines the treatment objective, anatomical limits, backup decisions if tissue response is weaker than expected, and the records needed if the patient later seeks revision or surgery elsewhere.
Vector planning should stay anatomy-led. Clinics commonly assess the direction of lift, fixed support regions, soft tissue density, retention points, and the relationship between entry points and visible contour change. The exact markings, thread type, and placement method should follow the product labeling, formal hands-on training, and the operator’s scope.
Documentation before treatment usually includes baseline photographs, relevant medical history, medications and supplements, prior aesthetic procedures, informed consent, labeled product details, lot numbers, and a written aftercare plan. If the clinic uses templates, they should still allow enough detail to record treatment zones and any variations from the original plan.
Prior threads matter. If a patient may later undergo facelift or neck surgery, accurate records of thread type, treatment areas, and dates can make later assessment easier. Earlier thread procedures may alter tissue planes or leave retained material that a future surgeon needs to know about.
- Confirm candidacy and goals.
- Review medical and treatment history.
- Take standardized photographs.
- Verify product, lot, and expiry.
- Document marking plan and zones.
- Issue written aftercare instructions.
- Schedule follow-up and escalation contact.
Procedure-Day Workflow for Clinics
A repeatable procedure-day workflow reduces preventable errors. The room, team, documents, and escalation supplies should be ready before skin prep or local anesthetic begins.
Most clinics use the same sequence: verify identity and consent, recheck exclusions, inspect sterile packaging, confirm product and lot information, review the planned vectors, photograph markings if that is part of the protocol, perform a time-out, and record any deviation from the original plan. This is also the right point to reconfirm who is supervising, who is documenting, and who will give aftercare instructions.
Do not treat manufacturer instructions as optional. Label-specific handling, insertion tools, storage parameters, and single-use rules can differ across thread systems. If a clinic offers more than one thread brand, separate preference cards and room checklists help prevent mix-ups.
Brand-name medical products should come through vetted distributors and verified supply channels.
From a procurement angle, traceability matters as much as technique. Clinics should be able to match each treated case to the exact product used, its lot number, the treating provider, and the post-procedure note. That record becomes important if the patient reports delayed asymmetry, extrusion, infection, or later seeks another facial procedure.
Teams comparing non-surgical options may also find it useful to review related modality overviews on Mesotherapy Workflow, PRP Therapy, and Filler For Clinics when planning treatment menus or combination pathways.
Aftercare, Recovery, and Early Complication Recognition
Recovery expectations should be explained in concrete terms. Mild swelling, bruising, tenderness, a pulling sensation, or transient irregularity can occur early, but the clinic should define what is expected, what should improve within the usual short follow-up window, and what requires urgent review.
Written aftercare should be simple and consistent. Most clinics advise patients on facial movement limits, pressure avoidance, cleansing, makeup timing, sleep positioning, activity restrictions, and when to call the office. The exact instructions should match the product labeling and the clinic’s documented protocol.
When to reassess quickly
Escalation should be prompt for disproportionate pain, blanching or dusky skin color, spreading erythema (redness), fever, drainage, rapidly worsening asymmetry, thread extrusion, persistent dimpling, or new sensory or motor complaints. Clinics do not need to overstate risks, but they do need a clear route for same-day review or specialist referral.
Complication management starts with recognition and documentation. Record onset, symptoms, exam findings, photographs, and what the clinic advised. If an outside surgeon or emergency clinician becomes involved, complete records help protect continuity of care.
Quick tip: Use one follow-up script for all thread cases so red-flag symptoms are never left to memory.
For comparison with other rejuvenation pathways that may have different downtime or tissue effects, see Non-Surgical Mesotherapy, Hyaluronic Acid, and Non-Surgical Aesthetic Trends.
Training, Scope, and Governance
Training is not just a product demonstration. Clinics that use PDO threads need structured education in facial anatomy, depth awareness, aseptic handling, consent, adverse-event recognition, and documentation. A short vendor session may introduce a device, but it does not replace scope review, supervised practice, and a written competency process.
Governance should define which providers may consult, who may treat, what supervision is required, and how revisions or complications are escalated. If your clinic operates across multiple states or sites, standardize the policy but validate local law before assuming roles are transferable.
Mint PDO thread training should be assessed like any other procedural onboarding. Ask whether the education includes anatomy review, supervised hands-on practice, contraindication screening, photography standards, informed consent, complication drills, and records management. If any of those elements are missing, the workflow is incomplete.
Where Threads Fit Relative to Other Minimally Invasive Options
Threads occupy a specific lane. They are usually considered when the clinic wants mechanical support and contour change, not only hydration, glow, collagen signaling, or volume replacement. That is why they are often discussed alongside, but not interchangeably with, fillers, biorevitalizers, PRP, mesotherapy, or energy-based devices.
In simple terms, PDO threads aim to reposition or support tissue. Fillers generally replace or redistribute volume. Skin boosters and mesotherapy focus more on skin quality and hydration. PRP is typically used for regenerative signaling rather than lift. Combination treatment plans may make sense, but sequencing should be deliberate and documented.
This provider model is limited to licensed clinic settings.
What to do next is operational. Decide whether your clinic needs a thread program at all, which provider types are eligible to train, how candidacy will be screened, and how complications will be triaged after hours. A smaller, better-governed service line is safer than a broader menu with weak oversight.
Authoritative Sources
- For device oversight and labeling context, see the FDA medical devices program.
- For published clinical literature searches, use PubMed.
- For specialty society education, review the American Society of Plastic Surgeons.
Further reading should focus on your exact thread system, your local scope rules, and your clinic’s written protocols for consent, documentation, and escalation.
This content is for informational purposes only and is not a substitute for professional medical advice.