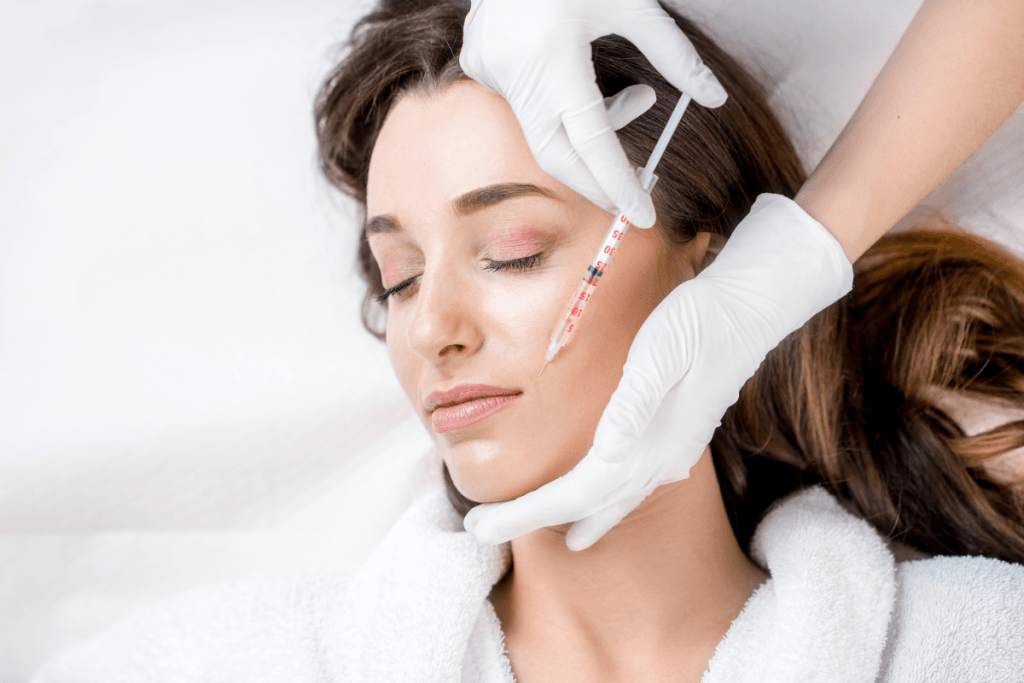
Key Takeaways
- Screen for infection, neuromuscular history, and prior toxin exposure.
- Standardize medication and supplement reconciliation to limit bruising.
- Set clear expectations on alcohol, exercise, heat, and skincare actives.
- Document indications, lot numbers, consent, and post-visit instructions.
Overview
For most aesthetic practices, what not to do before botox is less about “rules” and more about controlling variables that can affect bruising, swelling, and patient satisfaction. This page summarizes common pre-treatment avoidances and the rationale behind them, using clinical language and plain-language explanations your staff can repeat consistently.
It is written for clinic workflows, not consumer self-care. Where protocols vary, align your approach with your medical director and the product labeling. MedWholesaleSupplies supports licensed clinics with a B2B purchasing model, so the focus here stays on documentation, safety checks, and repeatable intake steps.
What Not To Do Before Botox in Clinic Workflows
Pre-treatment instructions work best when they match your intake process. Start by separating “must not” items (contraindications, infection at the site, incomplete consent) from “prefer not” items (modifiable behaviors that may increase bruising or transient swelling). That split helps front-desk staff triage calls without drifting into medical advice.
Next, decide what your clinic will document every time. Consistent charting reduces rework when patients return with concerns. If your practice also offers fillers, link neuromodulator intake to your broader injection safety SOPs, such as the guidance in Injection Safety for standard precautions and room setup.
Core Concepts
Botulinum toxin type A (neuromodulator) injections are brief, but the pre-visit details can drive outcomes. Patients often ask about alcohol, coffee, exercise, sleeping position, and skincare. Clinics also need a consistent approach to anticoagulants, antiplatelets, and OTC analgesics.
The concepts below can be converted into your handout, portal message, or pre-visit checklist. Use them as prompts for clinician review rather than fixed medical directives.
Medication Reconciliation and Bruising Risk
Many “what to avoid” conversations are really about ecchymosis (visible bruising). Bruising risk can increase with medications and supplements that affect platelet function or coagulation. That includes common OTC nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, as well as aspirin in some patients. It can also include prescription anticoagulants (blood thinners) and certain supplements.
Operationally, the key step is not telling patients to stop therapy. The key step is documenting what they took, why they take it, and who manages it. When someone asks about “tylenol before botox,” note that acetaminophen (Tylenol) is not an NSAID, but still route advice through the prescriber. Add a standard pathway for same-day disclosures, so staff know when to escalate to the injector.
Alcohol, Caffeine, and Hydration Conversations
Alcohol questions come up constantly, including “alcohol night before botox” and whether drinking changes results. Your pre-visit messaging can stay neutral: alcohol may increase flushing and can be associated with easier bruising in some people. Patients also ask, “can I drink coffee before botox,” often because they are worried about blood pressure or jitters during injections.
Rather than giving one-size limits, define what your clinic will document and what you will postpone for. For example, if a patient arrives visibly impaired or cannot consent, that is a safety issue. If they report routine caffeine intake, your team may simply note it and proceed. This approach keeps messaging consistent and reduces staff improvisation.
Skin Integrity, Active Dermatoses, and Skincare Actives
Before injection, skin condition matters. Screen for active dermatitis, sunburn, or local infection near the planned sites, since these may change the risk profile or require rescheduling. Patients also ask about a “skincare routine before botox,” especially when they use retinoids.
Retinoid (vitamin A derivative) products like retinol are common, and questions such as “why no retinol before botox” usually reflect irritation concerns, not toxin performance. The practical clinic issue is whether the skin is inflamed or sensitized on exam. If a patient asks “what happens if you use retinol before botox,” document use, check for erythema or peeling, and let the injector decide if technique or timing should change.
Exercise, Heat Exposure, and Scheduling Around Events
“Can I exercise before botox” is a scheduling question as much as a medical one. Some clinics prefer to minimize vigorous exercise and high heat exposure around injections, because increased blood flow and perspiration can worsen transient redness or swelling, and may contribute to bruising in susceptible patients.
From a workflow perspective, ask about same-day workouts, hot yoga, sauna use, and major events (weddings, photo shoots). Then document what you advised in plain language. This reduces after-hours messages about “I worked out and now I’m swollen,” and it standardizes expectations.
Positioning Myths and Real-World Counseling
Patients frequently search for “lying down after botox myth” and “how long after botox can I sleep on my side.” While your post-care handout should address positioning, pre-visit counseling can prevent panic. The goal is to set realistic expectations: people may inadvertently touch their face, nap, or lean on a pillow, and most concerns are about symptom monitoring and avoiding heavy pressure or rubbing.
Tip: Build a short script for staff who get the call, “I forgot and laid down after getting botox.” Train them to document timing, symptoms, and what area was treated, then route to the injector for individualized guidance.
When Botox Is Combined With Other Injectables
Patients also ask “what not to do before botox and fillers,” because many practices co-schedule services. The operational risk is not the combination itself. The risk is unclear sequencing, incomplete consent, and mixing aftercare instructions.
If your clinic commonly pairs treatments, keep a single “combined visit” instruction set. For broader sequencing considerations, see Botox And Fillers Combined as a planning reference, and align it with your own protocols.
Practical Guidance
Use the checklist below as a template for intake calls, pre-visit forms, and day-of huddles. It is intentionally conservative and documentation-focused. Adjust it to your jurisdiction, scope, and medical-director preferences.
Keep the language consistent across front desk, nursing, and injectors. Mixed messages are a common driver of complaints, especially around bruising, “coffee,” and OTC medications.
Pre-Visit Intake Checklist (Documentation-First)
- Confirm indication and sites: record intended areas and prior response history.
- Review contraindications: note neuromuscular conditions and prior adverse events.
- Assess skin status: document rash, sunburn, acne flares, or infection near sites.
- Reconcile meds and supplements: capture aspirin, NSAIDs, anticoagulants, and herbals.
- Substance use notes: document alcohol use the prior day if disclosed.
- Skincare products: record retinol/retinoid use and any irritation.
- Event timing: document upcoming photos, travel, or athletic events.
Standard “Do Not” Items Your Clinic Can Enforce
Some boundaries are operational and safety-based, and clinics can enforce them consistently. Examples include proceeding without valid consent, treating through visible infection at the site, or continuing when a patient cannot follow instructions. These items are less debated because they tie directly to safety and documentation.
Note: If your practice has a high volume of first-time patients, consider adding a short consent teach-back step to reduce misunderstandings about expected onset and the difference between neuromodulators and dermal fillers.
- No treatment without consent: ensure comprehension and capacity are documented.
- No injections through infection: reschedule if skin is compromised at planned sites.
- No same-day add-ons without review: keep changes within prescriber oversight.
- No conflicting aftercare sheets: provide one unified instruction set per visit.
How to Handle Common Patient Questions (Without Giving Medical Advice)
Staff can answer many questions by explaining “why we ask” and “what we document,” then escalating decisions. For “can I take ibuprofen before botox” or “can I take aspirin before botox,” the safest operational response is to capture the last dose, the indication, and the prescriber, then route the question. For “does drinking alcohol after botox make it less effective,” avoid efficacy claims and focus on bruise/swelling expectations and consent capacity.
For skincare questions like “how soon can I use retinol after botox,” keep the response tied to skin tolerance and irritation risk, not guarantees. For positioning questions like “how to sleep after botox in forehead,” confirm the clinic’s post-care instructions are being followed and document any pressure or rubbing. When in doubt, use your escalation pathway and chart the discussion.
Compare & Related Topics
Many searches bundle pre- and post-care. Your clinic handouts should clearly separate what not to do before versus what not to do after botox, because patients often mix the two. Pre-care is mostly about avoiding preventable bruising and ensuring safe consent. Post-care tends to focus on avoiding rubbing, monitoring symptoms, and following the injector’s technique-specific guidance.
It also helps to clarify how neuromodulators differ from fillers. Fillers add volume, while botulinum toxin modifies muscle activity. If your team wants a refresher on documentation and workflow expectations around injectables, Before And After Documentation provides photo and charting structure you can adapt, and Dermal Filler Injection Protocols summarizes safety steps that often translate to toxin visits.
For practices that offer multiple injectable categories, planning resources can reduce confusion when patients book “everything at once.” See Juvederm Clinic Workflow for an example of how clinics standardize counseling across products. For broader planning comparisons, Sculptra Versus Filler can help teams explain collagen stimulators versus HA fillers without overpromising outcomes.
Clinic Ordering and Compliance Notes
Stocking neuromodulators and injectables requires more than a purchase order. Set up a repeatable process for credential checks, lot tracking, and documentation retention. Ordering through MedWholesaleSupplies is restricted to licensed clinics and credentialed healthcare professionals, which supports controlled distribution expectations in clinical settings.
For adjunct procedures sometimes scheduled around neuromodulator visits, keep supply decisions tied to training and scope. If your clinic pairs fillers with other services, procurement references like Filler Sourcing Standards can be used to audit vendor documentation and reduce gray-market risk. MedWholesaleSupplies supplies brand-name medical products through vetted distributors and verified supply channels for licensed clinics, which can simplify internal compliance reviews.
- Verify eligibility: maintain current licenses and prescriber credentials on file.
- Document traceability: record lot numbers, expiry, and receiving dates.
- Standardize storage logs: align with manufacturer requirements and internal audits.
- Control inventory access: limit handling to trained staff with documented SOPs.
If your clinic also uses cannulas or microinjection devices in combined visits, link ordering to a procedure list approved by your medical director. Examples include Softfil Cannula for cannula-based filler technique support, or Fillmed Nanosoft Microneedles when your protocol includes superficial microinjections on separate days.
Authoritative Sources
Use product labeling and professional society guidance to anchor clinic policies, especially where patient instructions vary by technique and indication. For on-label contraindications and safety warnings, refer to the manufacturer’s prescribing information, such as BOTOX (onabotulinumtoxinA) Prescribing Information.
For general educational framing and risk counseling language, professional organizations can also help standardize patient expectations. One example is the American Society of Plastic Surgeons overview of botulinum toxin. Keep your final policy aligned with your medical director, local regulations, and the specific product used.
Recap: build a documentation-first intake, standardize messages on bruising risk factors, and separate pre-care from aftercare. That structure reduces variability across staff and improves follow-through.
This content is for informational purposes only and is not a substitute for professional medical advice.