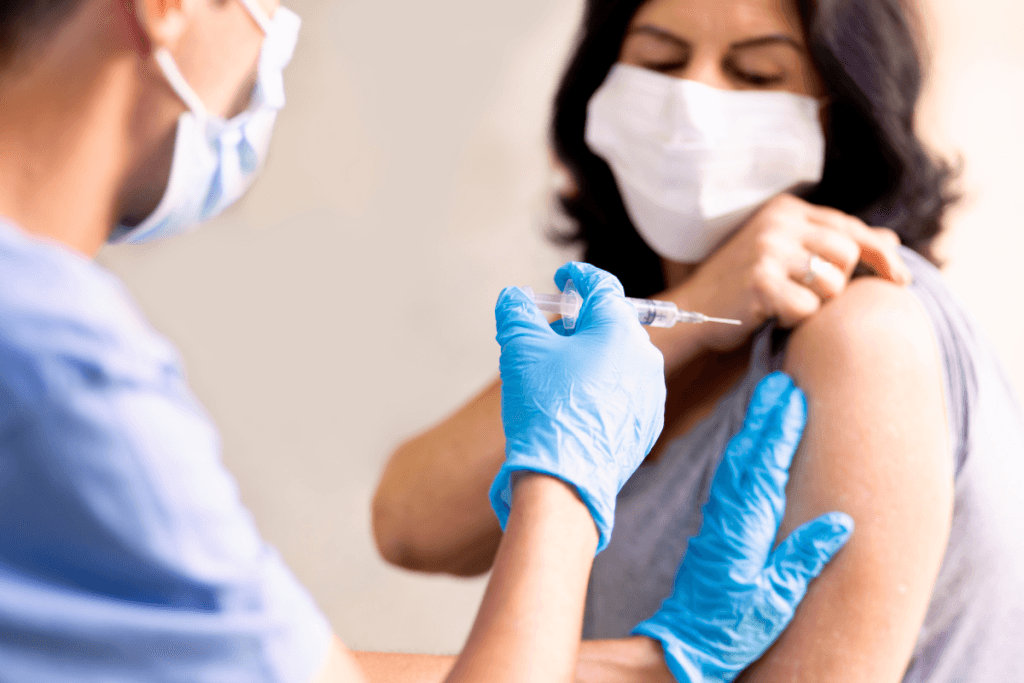
Evenity injection for osteoporosis is a clinic-administered romosozumab treatment that blocks sclerostin, a protein that suppresses bone formation. In practical terms, it works differently from standard antiresorptives because it can increase new bone formation while also reducing bone resorption. That matters when a clinic is evaluating postmenopausal osteoporosis with high fracture risk, prior fragility fracture, or poor fit with prior therapy. For healthcare teams, the core questions are usually who fits treatment, how monthly administration works, what safety checks matter most, and what should happen after the 12-month treatment window ends.
Key Takeaways
- Romosozumab is a sclerostin inhibitor with both bone-building and bone-loss slowing effects.
- U.S. use is generally limited to postmenopausal women at high fracture risk.
- Each monthly dose is given by a healthcare professional as two consecutive subcutaneous injections.
- Up-front review should cover cardiovascular history, calcium status, dental factors, and the post-treatment plan.
This page is written for licensed clinics and healthcare professionals.
Evenity Injection for Osteoporosis in Clinic Practice
At a high level, romosozumab is a time-limited anabolic biologic used when fracture risk is high enough that early bone-building effect may change the treatment conversation. It is not a universal first choice for every patient with low bone density. In the U.S., the approved use is for postmenopausal women with osteoporosis at high risk for fracture, including those with a history of osteoporotic fracture, multiple fracture risk factors, or failure or intolerance to other available therapy.
Who Is Typically Considered
In day-to-day practice, candidate review usually centers on fracture history, bone mineral density, prior osteoporosis treatment, renal considerations, adherence risk, and the urgency of reducing near-term fracture risk. Clinics often discuss romosozumab when they need more than a maintenance antiresorptive approach. It may fit patients who have already fractured, have very low bone density, or have not done well with other therapies. Final selection still depends on the prescriber, the full history, and local workflow.
Why it matters: The long-term plan should be mapped before the first dose because the course ends after 12 months.
That time-limited structure changes how clinics schedule follow-up. Instead of viewing the medication as open-ended maintenance, teams usually treat it as one phase of a larger osteoporosis pathway. That means front-end work matters: documentation, warning review, patient counseling, and planning the next medication before the last dose is due.
How This Sclerostin Inhibitor Works
Romosozumab works by binding to and inhibiting sclerostin, a protein that normally restrains bone formation. When that brake is reduced, osteoblast activity rises. Osteoblasts are the bone-building cells. At the same time, bone resorption also falls to a degree, which gives the drug a dual effect. That combination is what makes it distinct from therapies that mainly slow bone breakdown alone.
Clinically, that means teams can describe the drug as both anabolic and antiresorptive. Anabolic means bone-building. Antiresorptive means bone-loss slowing. Early in treatment, the bone-forming signal tends to stand out more strongly. Over time, the overall goal is better bone strength and lower fracture risk rather than symptom relief that a patient can feel right away.
Does It Build New Bone
Yes. Label-backed descriptions and major medical references describe romosozumab as increasing bone formation, not just preventing further loss. That is why it is often discussed differently from maintenance agents. Still, clinics should frame expectations carefully. Patients do not feel bone formation in the way they might notice pain relief from another class of therapy. Success is judged through fracture-risk context, adherence, and follow-up assessment rather than a quick subjective effect.
How Fast Can Effects Be Detected
Biologic activity may be detectable in bone turnover markers within weeks, but that does not make it an immediate symptom treatment. It is better framed as a structured osteoporosis therapy with early biologic effect and longer-horizon clinical goals. For staff education and counseling, it helps to separate the question of when the mechanism starts from the question of when bone density or fracture outcomes are reassessed.
That distinction also prevents overpromising. Clinics should avoid language that suggests a single monthly visit will produce a rapid, noticeable physical change. The more accurate message is that romosozumab begins acting on bone-remodeling pathways early, while treatment success is evaluated over the full course and beyond.
What Administration Looks Like in Clinic
Administration is straightforward, but it is not casual. Under the U.S. prescribing framework, each monthly dose consists of two consecutive subcutaneous injections given by a healthcare professional, and the full course is limited to 12 monthly doses. Evenity injection for osteoporosis is therefore a recurring clinic service line, not a one-time intervention and not an infusion.
Clinic Workflow Snapshot
- Verify indication — confirm high-fracture-risk context and prior therapy history.
- Review warning history — document recent myocardial infarction or stroke.
- Check calcium status — correct hypocalcemia before administration.
- Confirm dental context — note major procedures and jaw-risk factors.
- Prepare monthly visit — administer two consecutive subcutaneous injections.
- Record follow-up plan — map the transition before dose 12 is completed.
Operationally, the monthly cadence affects scheduling, inventory handling, and continuity tracking. Missed visits can disrupt the intended treatment sequence, so many clinics build reminder and documentation steps into the visit workflow. It also helps to standardize where counseling is documented, who confirms warning review, and how the next-phase therapy discussion is recorded.
Teams that manage both injections and infusion services may find it useful to contrast this workflow with infusion-based pathways. For related clinic context, see Bone Infusion Uses and Infusion Side Effects. The documentation needs overlap in places, but the administration model is different.
Supply discussions here assume vetted distributor channels for licensed clinics.
Safety, Monitoring, and Practical Cautions
Safety review starts with cardiovascular history. The prescribing information warns against initiating romosozumab in a patient who has had myocardial infarction (heart attack) or stroke within the preceding year. Beyond that, clinicians may still weigh overall cardiovascular risk when deciding whether the mechanism and treatment window fit the case. For clinics, Evenity injection for osteoporosis usually warrants a more deliberate pre-start screen than a routine maintenance injection.
Hypocalcemia (low calcium) is another key issue. It should be corrected before treatment begins, and clinics often pay closer attention when severe renal impairment is present because calcium disturbances may be more likely. Commonly discussed adverse effects include arthralgia, headache, and injection-site reactions, but those should not overshadow the more important warning review. For a deeper internal summary, see Evenity Side Effects.
Dental history also matters. Osteonecrosis of the jaw, a rare jawbone complication, has been reported with antiresorptive and anabolic bone therapies, including romosozumab. That does not mean every patient needs the same dental pathway, but it does mean clinics should document active dental problems, recent invasive dental work, and counseling around oral symptoms. New thigh or groin pain also deserves attention because atypical femoral fracture, while uncommon, has been reported.
Hypersensitivity is another practical counseling point. Staff should know how the clinic escalates rash, swelling, breathing symptoms, or other reactions that raise concern for allergy. Local protocols vary, but the broader principle is simple: warning review should happen before the injection encounter, not after a problem appears.
Quick tip: Use one pre-dose checklist each month so cardiovascular, calcium, and dental questions are reviewed the same way every time.
After Month 12: Planning the Next Phase
The treatment course stops after 12 monthly doses. That limit is central to the product’s place in care. Romosozumab is designed as a defined anabolic phase, not indefinite treatment. Once that phase ends, bone-density gains may not be maintained as well if care simply stops without a follow-on plan.
That is why clinicians often line up an antiresorptive agent before the final months of therapy are completed. Antiresorptive means a treatment that mainly slows bone breakdown. The exact next step varies by patient history, renal considerations, prior exposure, adherence factors, and prescriber judgment. In clinic workflow terms, month 10 or 11 is often when teams confirm documentation, coverage requirements, imaging plans, and the intended handoff so the final dose does not become an operational dead end.
Denosumab is one common follow-on discussion point, although it is not the only one. For additional internal background, review Prolia Injection. The larger principle is that the first dose of romosozumab should never be separated from the end-of-course transition plan.
How It Compares With Other Osteoporosis Injection Options
The main difference is mechanism. Compared with maintenance antiresorptives, Evenity injection for osteoporosis is usually framed as a front-end, time-limited therapy that both builds bone and slows resorption. Denosumab and bisphosphonates, by contrast, are mainly antiresorptive strategies. That does not make one class universally better. It means they solve different treatment problems.
| Therapy or Class | High-Level Mechanism | Typical Place in Care | Clinic Note |
|---|---|---|---|
| Romosozumab | Blocks sclerostin and increases bone formation while reducing resorption | Time-limited option for very high fracture risk in approved use | Requires monthly clinic administration and a post-12-month transition plan |
| Denosumab | Antiresorptive therapy that reduces osteoclast-driven bone breakdown | Common maintenance option in osteoporosis care | Continuity matters because stopping therapy needs a clear follow-up strategy |
| Bisphosphonates | Antiresorptive class that slows bone turnover | Often part of first-line or follow-on treatment pathways | Route, renal fit, and adherence issues vary across agents |
In practical decision-making, clinics usually compare these options across four factors: fracture urgency, prior treatment response, safety profile, and what the patient can realistically maintain over time. For a focused comparison, see Evenity vs Prolia. For broader denosumab context, review Prolia Bone Health.
The other important distinction is service design. Romosozumab creates a defined monthly workflow with a fixed endpoint, while other therapies may fit longer maintenance models. That difference affects scheduling, documentation, and patient counseling just as much as it affects mechanism-of-action discussions.
Brand-name products should move through verified supply pathways.
Authoritative Sources
- For the official U.S. label, see the FDA prescribing information for Evenity.
- For specialty-society background, review the American College of Rheumatology page on romosozumab.
- For general drug reference details, see MedlinePlus information on romosozumab injection.
In clinic practice, the key question is not only whether romosozumab works. It is whether the patient fits the approved high-risk setting, the warning review is clear, the monthly workflow is dependable, and the post-treatment transition is already planned.
This content is for informational purposes only and is not a substitute for professional medical advice.