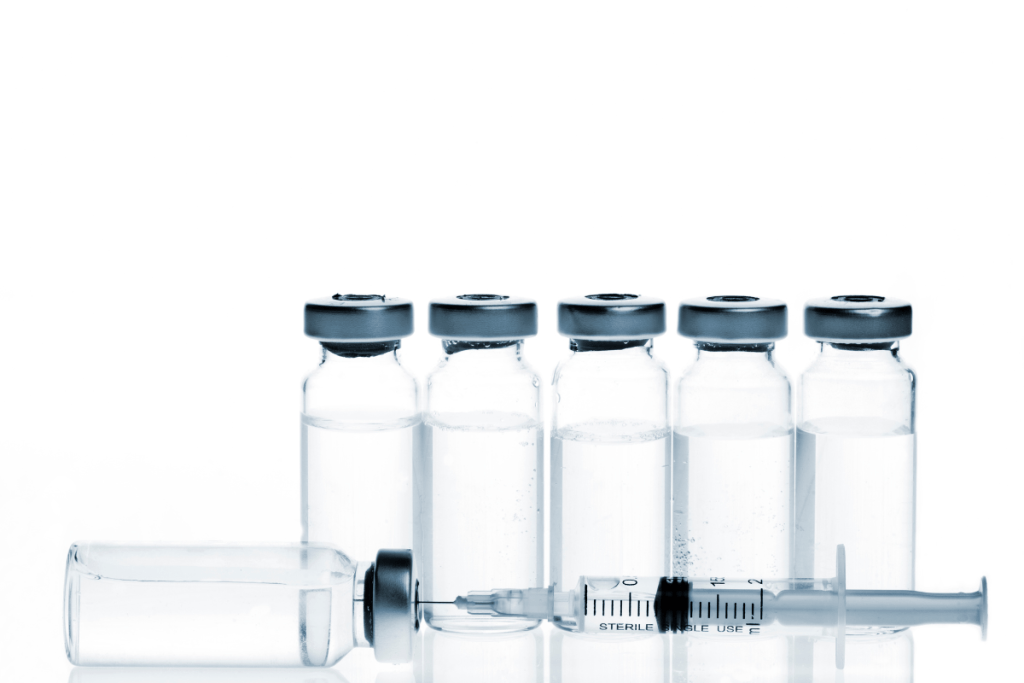
Proper neurotoxin storage is a cold-chain discipline, not a shelf habit. In practical terms, How to Store Botox for Clinics: Handling and Stability means keeping each vial within the label-specified temperature range, verifying conditions at receipt, separating unopened from reconstituted stock, documenting excursions, and training staff to follow one consistent workflow. That matters because botulinum toxin products are sensitive biologic preparations. Small handling errors can affect stability, create avoidable waste, and complicate traceability during an audit or adverse-event review.
Key Takeaways
- Use the current package insert for the exact product and presentation in hand.
- Separate unopened inventory from reconstituted stock and quarantine any questionable vial.
- Build storage SOPs around receipt, refrigeration, monitoring, labeling, and documentation.
- Do not assume one neurotoxin brand follows another brand’s storage language.
- Escalate temperature excursions through documented review, not visual guesswork.
Why Storage Affects Stability and Workflow
Storage errors matter because botulinum toxin products are temperature-sensitive biologics. Many are supplied as lyophilized (freeze-dried) material before preparation. Their condition may not be obvious by sight alone. A vial can look normal after avoidable heat exposure, a delayed handoff, or incomplete monitoring. That is why clinics need a process that covers transport, receipt, refrigeration, preparation status, and quarantine decisions.
For teams that manage several injectable products, the storage issue is not only scientific. It is operational. One missed receiving check can disrupt a treatment list, trigger replacement work, and force retrospective record review. If your inventory spans multiple products in the Botulinum Toxins Category, it helps to treat neurotoxin storage as part of the same quality system you use for lot tracking, expiration review, and procedural documentation.
Unopened Botox storage and reconstituted Botox storage are also not the same question. Before preparation, the focus is labeled temperature control, protected placement, and stock rotation. After reconstitution, the focus shifts to time marking, separation from unopened vials, and strict adherence to the product-specific instructions for use. Keeping those two states distinct reduces confusion during busy clinic sessions.
This site is structured for licensed clinics and healthcare professionals.
Botox Storage Guidelines Start With the Product Label
The safest storage rule is to follow the current package insert for the exact brand, market, and presentation in hand. That sounds basic, but it is where many clinic errors begin. Teams often remember a general refrigeration rule and then apply it across products, lot sizes, or geographies. In practice, official labeling may differ on unopened storage, post-reconstitution conditions, handling language, or how long a prepared vial may remain suitable under specified conditions.
If you carry more than one toxin, create a product matrix instead of relying on memory. A simple matrix can pull the storage language from the Botox Product Page, the Dysport Product Page, and your internal SOP. The same principle applies when you review the broader Botulinum Toxins Product Hub before updating clinic protocols. One refrigerator can hold several neurotoxin products, but it should not blur the distinctions between them.
Unopened stock needs controlled placement
Unopened vials should stay in the location and condition stated in the current labeling. For most clinics, that means prompt placement in the correct refrigerated environment, limited handling, and clear separation from non-medication items. It also means preserving carton information when that packaging supports identification, traceability, or light protection. Stock rotation should follow FEFO, or first-expire, first-out, so older but still acceptable inventory is used before newer lots.
Reconstituted stock needs tighter oversight
After reconstitution, the risk profile changes. The clinic must now manage both temperature and time, along with clear labeling of preparation status. A ready-to-use vial should never drift back into the unopened bin. It should carry the date and time of preparation, any staff identifiers required by policy, and a clear signal that it belongs to the reconstituted workflow. If any of those details are missing, staff should not improvise.
Why it matters: A vial’s appearance cannot confirm that labeled storage conditions were maintained.
Receiving, Refrigeration, and Daily Handling
Most storage failures happen at handoff points, not while a vial sits untouched. Delivery, intake, refrigerator access, and end-of-day cleanup are the usual weak spots. That is why Botox refrigeration requirements should be built into a receiving routine, not left to whoever happens to sign for the shipment. If your practice is refining broader injectable operations, Facial Aesthetic Planning offers a useful workflow lens for where storage controls belong.
When a shipment arrives, the receiver should inspect the parcel condition, verify that any temperature-control measures appear intact if they were used, record the lot number and expiration date, and move product promptly to the correct storage area. That sequence protects both the product and the record. It also limits the common gap between delivery and refrigeration that creates uncertainty later. A quick intake log is often more valuable than a long narrative written days after the fact.
Daily refrigeration control also needs structure. Clinics should assign responsibility for temperature monitoring, define where neurotoxin products are stored, and keep that location orderly enough that staff can find one vial without warming the entire shelf. Overstocking, crowding, and frequent door opening can undermine stability. The same is true when products with different handling states are mixed together. For procurement teams reviewing supply chain discipline across injectables, Sourcing Standards is useful background on why verification and documentation matter before a product ever reaches the treatment room.
| Scenario | What to verify | Why it matters |
|---|---|---|
| After delivery | Parcel condition, lot, expiry, and prompt transfer to storage | Confirms chain of custody from receipt onward |
| Unopened vial in storage | Correct temperature range, organized placement, and FEFO rotation | Reduces waste and retrieval errors |
| Prepared vial | Preparation time, status label, and physical separation from unopened stock | Prevents mix-ups during treatment flow |
| Temperature excursion | Quarantine, documented temperatures, affected lots, and review path | Supports safe disposition and audit readiness |
Listed products are sourced through vetted distributors and verified supply channels.
What Changes After Reconstitution
Once a neurotoxin is reconstituted, the operational margin usually narrows. The clinic is no longer managing only unopened inventory. It is now managing a prepared biologic with label-specific storage language, a shorter usable window where applicable, and more opportunity for staff confusion. This is where Botox handling and stability become a matter of disciplined labeling and limited assumptions.
The key question is not whether a clinic usually refrigerates prepared product. The key question is what the exact product labeling allows after reconstitution and how your policy operationalizes that instruction. Teams should mark the preparation time clearly, segregate prepared vials from unopened stock, and avoid carrying uncertain items forward into later sessions. If the reconstitution status, timing, or storage condition cannot be confirmed, the vial should be treated as unresolved until reviewed under policy.
This product-specific approach also matters in mixed-brand practices. A clinic that stocks Bocouture Product Page inventory or reviews the Azzalure Product Page alongside other toxins should document each product’s handling language separately. A shared refrigerator does not create a shared rule set. It only increases the need for precise, visible differentiation.
Handling Temperature Excursions and Quarantine Decisions
A temperature excursion should trigger quarantine and documentation, not guesswork. Clinics cannot reliably judge a neurotoxin vial’s suitability by appearance alone after a storage problem. If the refrigerator drifts out of range, a parcel sits too long before intake, or monitoring data are incomplete, the affected product should be physically separated from active inventory until the issue is reviewed against the current labeling and the appropriate escalation path.
A practical excursion record usually includes the date and time the issue was discovered, the known or estimated duration, the highest and lowest observed temperatures if available, the affected lot numbers, where the product was stored, and who reviewed the event. It should also record the disposition decision. That may involve consultation with the manufacturer, the authorized supplier, or internal quality leadership, depending on the product and clinic structure. What matters is that the decision is documented and reproducible.
- Quarantine first and label the hold area clearly.
- Capture the affected lot and expiry details.
- Record the observed temperature data available.
- Review current labeling before releasing any stock.
- Document the final disposition and rationale.
Quick tip: Keep quarantine stock physically separate from routine refrigerator inventory.
Teams should also review why the event occurred. A recurring excursion often points to a workflow gap, such as shared refrigerator access, missing backup coverage, late deliveries, or unclear intake ownership. Corrective action does not need to be elaborate. It does need to be written, assigned, and checked.
A Practical Storage Workflow for Clinics
A short written workflow reduces variation across injectors, assistants, and front-desk receivers. This matters in aesthetic practices, licensed medical spas, and multi-provider clinics alike. The aim is not bureaucracy. The aim is a repeatable storage pathway that any trained team member can follow when the primary injector or manager is unavailable.
- Assign one receiving owner and one backup.
- Inspect deliveries immediately on arrival.
- Record lot and expiration at intake.
- Place vials promptly in the designated storage location.
- Separate unopened, prepared, quarantined, and expired items.
- Review logs on a defined routine.
- Retrain staff after any deviation or near miss.
Clinics often do well with a one-page refrigerator reference sheet. It can list each neurotoxin product stocked, the storage state being managed, where it belongs physically, who to contact during an excursion, and which document holds the current label language. That approach is especially helpful when a clinic rotates staff across sites or adds new brands over time.
Botox storage after delivery should also be included in this workflow. The receiving step is where cold chain management is either preserved or weakened. If your process begins only once the carton reaches the refrigerator shelf, it begins too late.
Managing Multiple Neurotoxin Brands Without Mixing Rules
Multi-brand inventory adds complexity because storage assumptions do not always transfer. A clinic may stock Botox for some sessions, review Dysport for others, and consider alternatives such as Bocouture, Azzalure, or Xeomin Product Page inventory depending on availability and practice patterns. The operational mistake is to flatten those products into one remembered rule.
A better approach is to standardize the framework while keeping the product details distinct. The framework can stay constant: verify on receipt, refrigerate as labeled, track lot and expiry, mark preparation status, quarantine excursions, and document disposition. The details must stay product-specific: the exact storage language, the allowed conditions after reconstitution, and any presentation-specific handling notes in the current labeling.
This distinction helps both clinicians and procurement teams. Clinicians avoid treatment-day uncertainty. Operations staff avoid preventable waste. Practice managers get cleaner documentation. And quality reviews become faster because the team can show not only what happened, but also which product-specific instruction governed the decision.
Authoritative Sources
For current storage language, use official labeling and regulator-backed references rather than memory, training slides, or old SOP copies.
- AbbVie Botox Cosmetic Prescribing Information
- FDA Drugs@FDA Labeling Database
- DailyMed Drug Labeling Database
In day-to-day practice, How to Store Botox for Clinics: Handling and Stability is less about memorizing one number and more about running a reliable, label-driven process. If your clinic documents receipt, separates product states clearly, monitors refrigeration consistently, and escalates deviations through a written pathway, storage decisions become easier to defend and easier to repeat.
This content is for informational purposes only and is not a substitute for professional medical advice.